BackReviver Posture Support Back Brace
- Designed for posture‑related lower and mid‑back pain that builds with long sitting or standing and eases when you move.
- Firm lumbar belt with semi‑rigid stays and pad to support the lower back, limit sharp bends and control twisting without locking you solid.
- Full‑length back panel with shoulder straps to support the upper and mid‑back and gently guide the shoulders away from rounded‑shoulder and sway‑back postures.
- Front‑fastening, adjustable design so you can set a firm, even hold for busier periods, then ease it off when you are resting.
- Slim enough to sit under most everyday clothing, with breathable materials for use during work, travel and light activity.
- Built‑in magnets over the upper and lower back as a comfort feature for some users (not suitable with implanted electronic or magnetic devices, or during pregnancy).
Who this posture support back brace is for
Many people live with back pain that is clearly linked to posture and time in one position. It may be fairly settled when you start your day, then gradually stiffen and ache as you sit at a desk, stand in queues, drive, or repeat the same bends and reaches. A short walk or change of position often eases things for a while, but the discomfort returns when you slip back into the postures that tend to cause trouble.
This pattern is often called mechanical or posture‑related back pain. It usually feels:
- worse the longer you sit or stand in one way,
- clearly aggravated by deep slumps, strong backward arches or awkward twists,
- at least partly relieved when you move, change position or stand up and walk.
If you recognise this description of your back pain, this is the sort of pain this BackReviver brace is designed to help you manage in everyday life.
It is intended for adults who:
- have ongoing or recurrent upper, mid‑ or lower‑back pain that clearly worsens with time spent in one position,
- notice that slumping forwards, over‑arching the lower back or twisting awkwardly tend to bring symptoms on,
- have tried lighter posture reminders or very soft supports and feel they now need something more structured around the lower back,
- want help to keep a more comfortable, fairly straight posture while they stay active and work through an exercise or rehabilitation plan.
This brace is not the first step if you have sudden, severe, unexplained back pain, new nerve symptoms such as leg weakness or loss of bladder or bowel control, or a suspected fracture or serious disease. Those situations need medical assessment before you consider using a brace.
What is happening in your back when posture causes pain
Each level of your spine is made up of:
- a block of bone at the front (the vertebral body),
- a disc between the vertebrae,
- a pair of small joints at the back (facet joints),
- and the ligaments and muscles that support and control movement.
When you sit or stand in a reasonably upright position and move often, the load is shared between these structures and they usually cope well. When you spend long periods:
- sitting or standing very rounded forwards, or
- standing with a strong arch in the lower back,
the same areas are compressed or stretched for too long and muscles have to work harder just to hold you up.
In these long‑held or end‑of‑range postures:
- the discs can be put under uneven pressure, especially at the back‑outer rim,
- the facet joints can be jammed together or pulled apart at their limits,
- ligaments and joint capsules can be held at, or beyond, the end of their comfortable range,
- and muscles can end up doing more “holding work” and less healthy movement.
That is why those postures may feel fine at first, but then start to hurt or feel tiring if you hold them for too long. Over weeks and months, many people respond by moving less and tensing more, which can weaken muscles and make each flare‑up last longer or come back more often.
Over a typical day, posture often changes gradually rather than in one sudden shift. You might start the day sitting or standing in a fairly good position. As you focus on work, reading, driving or other tasks, attention moves away from your body. The head begins to drift forwards, the shoulders round, or the hips move forwards and the lower back arches more. These head‑forward and sway‑back positions put more uneven load on the discs, facet joints and supporting tissues described above. As supporting muscles tire, your body tends to settle into the position that feels easiest at the time — often a slump or a heavily arched stance. Over hours, joints and discs then spend more time at the limits of their comfortable movement and muscles do more “holding” and less healthy movement. This helps explain why your back can feel so tired by the end of the day.
Once you can see how posture and everyday loading affect these structures, it becomes clearer why a few simple changes usually help — even before you add a brace.
What usually helps posture‑linked back pain before you think about a brace
Most people with ongoing or recurrent mechanical back pain do better with a mix of simple, consistent measures rather than relying on any single product.
It usually helps to stay as active as you reasonably can, rather than stopping completely every time the pain appears. Gentle walking and regular movement generally suit joints, discs and muscles better than long spells of stillness, even if you need to move more carefully for a while.
Breaking up long periods of sitting or standing with short, frequent changes of position also makes a difference. Standing up, walking to another room, or gently changing how you sit every 20–30 minutes can stop any one part of your spine being held compressed or stretched for too long.
Looking closely at how your work and home spaces are set up is often worthwhile and can reduce how sore or tired your back feels by the end of the day. Simple posture and set‑up changes — such as adjusting your chair height, using the chair’s backrest or a simple cushion for support rather than perching at the front of the seat, bringing screens up towards eye level, and placing frequently used items within easy reach — all make it easier to hold a comfortable, fairly upright posture rather than sliding into a deep slump or sway‑back.
The way the muscles around your spine and hips work together also makes a real difference. Exercises that help the deep abdominal and back muscles switch on and coordinate, along with work for the buttock and hip muscles, allow those muscles to share more of the everyday load so that sore joints and discs are not doing all the work. A physiotherapist or similar clinician can help you choose a simple set of exercises that matches your current level.
In some cases, short‑term pain relief or simple heat or cold, if a clinician suggests it, can make it easier to move and exercise while you work on these underlying issues.
Taken together, these steps reduce the extra strain on sore structures and change how your spine is loaded through the day, so the same areas are not always taking the most pressure. You do not have to make every change at once. It is usually better to start with a few manageable changes that you can keep up, rather than trying to change everything at the same time.
These are the basics to have in place alongside any support such as a brace. A brace like the BackReviver is there to support these changes and help you hold on to better positions and movement patterns during the parts of the day and the tasks you already know tend to make your back pain build.
How a posture support back brace can help
A well‑designed posture support brace can help posture‑related mechanical back pain in two main ways.
First, it provides a firm, adjustable hold around your trunk. Over the lower back, this can reduce sudden, sharp movements at irritated levels and make it harder to drop into your deepest bends and arches, without stopping you moving altogether. In simple terms, it nudges you towards the comfortable middle of your movement rather than the extremes that usually cause trouble.
Second, it acts as a physical reminder. As you start to slump forwards or arch backwards more than usual, you feel the brace press or tighten a little in certain areas. That prompt encourages you to bring your chest, head and pelvis back towards a more neutral, comfortable line before you sink fully into the positions that tend to wind your pain up.
A good brace should make it easier for your own muscles to work, not take their job away. You should still be able to breathe easily and walk, sit, stand and move in a natural way. The BackReviver brace takes these basic ideas further with firmer lumbar support and upper‑back guidance, which are described in the next section.
What this BackReviver brace is designed to do for you
This BackReviver Posture Support Back Brace is one of the firmer supports in the BackReviver range. It is for adults with posture‑related mechanical back pain — the sort of pain that builds with long sitting or standing and eases when they move — who need more than a very soft or minimal support but do not need a rigid brace.
It combines a structured lumbar belt, semi‑rigid stays, a full‑length back panel and adjustable shoulder and side straps. Each part has been chosen to change how your spine is loaded and moved in everyday positions, so you can spend more time in postures your back tolerates and less time in the ones that keep causing trouble. The overall design follows the same mechanical principles clinicians look for in a good back support: sharing load across the lumbar region, limiting extreme bends and arches, and giving gentle cues towards a more comfortable, sustainable posture.
Support for the lower back: belt, pad and semi‑rigid stays
Around your waist, the brace has a broad belt with a built‑in pad over the lower‑back region and slim, semi‑rigid stays inside. This gives firmer, more structured support to the lumbar spine than a simple elastic garment.
Mechanically, this:
- spreads contact across the lower back so one sore spot is not taking all the load,
- adds light compression, which can make the area feel more contained and less vulnerable,
- limits how far and how quickly you can bend or arch at the lumbar spine, without stopping you moving altogether.
When you bend forwards — for example to load a dishwasher, tie laces or pick up light objects from the floor — the stays and pad slow and limit the very deepest part of that bend. When you lean backwards or stand with your hips pushed forwards, the belt and stays resist the end of that arching movement and nudge you back towards a more comfortable middle position. Small, sudden sliding movements between vertebrae are reduced, which can be helpful if local joints, discs or ligaments at one level are irritable.
For many people, this lumbar section is what makes the brace feel noticeably different from a very soft or minimal support, such as simple elastic garments or thin posture straps: it does not lock you solid, but it provides a clear sense that your lower back is being guided and supported.
Support for the upper and mid‑back: full‑length panel and shoulder straps
Unlike supports that only cover the lower back, this brace has a padded panel running up the middle of your back and straps that come over the shoulders and around the sides of the chest. The aim is to support both the lower and mid‑back and to guide shoulder and upper‑back posture without a bulky front panel.
Mechanically, this:
- gives broad contact along the spine between the shoulder blades as well as in the lumbar area,
- encourages the shoulders and upper back to sit in a more natural line over the pelvis, rather than rounding forwards,
- provides gentle feedback when you start to slump, as the panel and straps tighten slightly and prompt you to bring your chest and head back.
In everyday use, this often makes it easier to avoid sliding into a deep rounded posture at a desk or when standing talking. It can reduce the effort your upper‑back muscles have to put in just to keep your head and shoulders reasonably upright, and soften the rounded‑shoulder, head‑forward posture that often goes with long hours at a desk or with kyphosis‑related ache.
Because there is no solid padded panel across the front of the chest, your chest and upper abdomen remain open. You can breathe easily and move your arms for everyday tasks and light activity, and the brace can usually sit under ordinary clothing without feeling bulky at the front.
Even, adjustable hold from front‑fastening straps
The main belt fastens at the front with a hook‑and‑loop closure, and there are extra side straps that you pull in from each side to increase or reduce tension. All adjustments are made from the front, so you do not have to twist to tighten it.
This arrangement lets you:
- set a snug, even hold around the waist, rather than a tight spot on one side,
- match the support to what you are doing — a little firmer for a long spell of sitting or standing, a little looser for rests and exercises,
- put on and adjust the brace yourself without awkward twisting.
You might fasten the belt and gently tighten the side straps before a block of desk work, a car journey, or a period of standing at a counter, then ease the straps off again when you sit for a rest, walk around more freely, or do your exercises, while still keeping some gentle posture cues from the back panel.
The idea is not to keep the brace very tight from morning to night, but to use the adjustability so you can support your back most during the parts of the day that usually cause problems.
Firm where you need it, flexible where you do not
This brace sits between very light strap‑only posture aids and rigid medical immobilisation braces. It is designed to be firm where most people with mechanical back pain need it — around the lower back — and more flexible higher up.
- In the lumbar area, the semi‑rigid stays and broad belt give a more structured hold. They are stiff enough to resist deep bending and arching, but flexible enough to allow normal walking, sitting and turning.
- In the upper‑back and shoulder region, there are no rigid stays. The panel and straps can move with your upper spine and ribs, so you can breathe and move your arms for everyday tasks and light activity.
This combination is intended to give the lower back enough guidance to feel steadier during sitting, standing and light activity, without the “locked‑in” feeling that would not be suitable for day‑to‑day use. It is not stiff enough to replace braces prescribed after surgery or fracture; it is for adults who need firmer guidance than a thin posture strap, but who still need to move freely.
Shaped to follow your back without digging in
Comfort where the brace touches your body is as important as the amount of support it gives. This design uses a slim, padded back panel and contoured straps to follow the natural curves of your spine and shoulders.
Key comfort details include:
- a padded panel along the spine and between the shoulder blades, which spreads contact over a larger area to reduce pressure points,
- shoulder and side straps that run over the tops of the shoulders and around the sides of the ribcage, away from the most sensitive parts of the underarm,
- a belt that sits at the narrowest part of the waist rather than cutting across the lower ribs or hips, with finished edges to reduce rubbing.
These details are there to reduce the chance of the brace cutting in at the edges when you move around, to limit rubbing or pressure marks over bony areas, and to make it easier to tolerate the brace for the periods of time when you most need extra support.
Designed to sit under everyday clothing
The materials used in this brace are chosen to be supportive but reasonably slim. The aim is that you can wear it under most ordinary tops, shirts or jumpers without it feeling bulky or obvious, which can matter if you want to use it at work or socially.
- The main body of the brace can usually be hidden under workwear or casual clothes.
- The fabric is reasonably breathable and quick‑drying, helping to reduce overheating and dampness under the brace.
- You can wear it for the active parts of your day — walking, doing household tasks, going up and down stairs — without it feeling heavy or overly warm.
It is not a replacement for supports designed for high‑impact or contact sports, but its relatively slim build and breathable materials mean many people can use it during light exercise such as brisk walking, and during ordinary working days, without it getting in the way.
Provides soothing magnetic comfort (with important safety limits)
This brace contains inbuilt magnets positioned along the mid‑back and within the lower‑back pad, roughly over the areas where many people report day‑to‑day soreness.
- The main structural support comes from the panel, belt and stays.
- The magnets are a comfort feature. Some people describe a calm or soothing sensation around those regions when using a magnetic support. Any such effect is individual and should be seen as an addition to, not a replacement for, the structural support the brace provides.
- The magnets do not touch the skin directly.
Because of the magnets, this brace must not be used by anyone with:
- a pacemaker or implantable defibrillator,
- a cochlear implant,
- an insulin pump, neurostimulator or any other implanted electronic or magnetic device.
The magnets are also one reason this brace is not suitable during pregnancy. If you are unsure whether the magnets are appropriate for you, check with a clinician before using this design.
Sized so the support sits where it should
This brace comes in several waist sizes and is shaped so that, when the right size is chosen, the back panel can support both the lower and mid‑back rather than only one small area.
The sizing chart is based on waist measurement, with approximate height ranges to help you judge how the panel will sit. If you are shorter, the right size makes it more likely that the panel will still reach up to around the shoulder‑blade area without digging into the back of the neck. If you are taller, the appropriate size should cover the lumbar spine and mid‑back, rather than stopping too low over the pelvis or only supporting a narrow band.
The waist measurement is the most important guide when you choose a size. In practice, choosing the right size and adjusting the belt and shoulder straps so the shaped back panel sits correctly is intended to make sure the brace supports the key areas of your back in line with these principles:
- covering the main lower‑back region where posture‑related mechanical pain is commonly felt,
- and allowing the upper panel to reach far enough to give useful upper‑back guidance, without being so tall that it rubs against the neck.
Taking a moment to measure and choose the right size helps the brace sit where it should and do its job properly for you.
How this brace relates to specific back conditions
Posture‑related mechanical back pain can come from several overlapping problems in the spine and pelvis, such as disc‑related pain, wear and tear in the facet joints, sacroiliac joint irritation, extra or poorly controlled movement at one spinal level, or a slip between vertebrae. The same design features in this brace — firm lumbar support, upper‑back guidance and adjustable control of bend, arch and twist — can help in slightly different ways in each of these problems, depending on which structures are most sensitive for you.
The condition overviews below describe how your pain may behave in common back‑pain patterns and how this brace may fit into managing each of them. They are not a diagnosis, but they may help you see how this design could apply to your particular pattern of pain.
For Back Strains and Sprains
What a back strain or sprain usually feels like
Back strains (in muscles and tendons) and sprains (in ligaments) are among the most common causes of sudden back pain. They often follow an awkward or heavy lift, a quick twist while reaching, or a burst of bending and carrying after a quieter spell. Pain may start at the time, or become more obvious later that day or the next morning. It is common to say the back has “gone” or “pulled”, and for certain movements to feel sharply painful or unsafe in the first few days.
People with this pattern often notice:
- a sudden, sharp pain at the time of injury, or a strong ache that builds later,
- pain and tightness when you try to bend, straighten or twist,
- difficulty getting in and out of bed, chairs or the car,
- a feeling that the back might “spasm” or “lock” if you move in the wrong way,
- and a tendency to hold yourself very stiffly in case “one wrong move” sets it off again.
If you recognise these features, this overview can help you understand what is usually happening in the muscles and ligaments, what tends to make things worse, and how this brace may fit into your recovery.
What is happening in the tissues
In a strain or sprain:
- some of the small fibres in the affected muscle, tendon or ligament are overstretched or torn,
- the body responds with inflammation — more blood flow and local activity to start repairing the damage,
- muscles around the injured area tighten to guard it, which adds to stiffness and the sense of the back being “locked”.
These changes make the area sensitive, especially when you move into your very deepest bends or twists. That is why the same simple movement can feel fine in a small range, then suddenly “grab” or feel sharply wrong if you push a little further. At rest, or with gentle movement in a comfortable middle part of your movement — not fully bent forwards and not fully arched backwards — you often feel a dull ache and stiffness that eases once you “warm up”.
Who tends to get these injuries
Simple back strains and sprains are very common in adults, particularly in people who:
- carry and lift heavier or awkward items at work or at home,
- sit for long periods and then tackle heavy or repetitive chores without building up gradually,
- have let general strength and conditioning drop,
- have had previous back injuries and gone straight back to full load.
Most people will experience at least one such episode; many will have several over a lifetime.
How this affects daily movement and why it can drag on
In the first few days, a back strain or sprain can make bending, straightening and turning feel very limited. Dressing, getting in and out of bed, picking things up from the floor and standing still for long can all be uncomfortable. A short reduction in heavy activity is appropriate right after the injury, but staying very still for long periods usually delays recovery.
If you hardly move, muscles weaken and tighten, joints and soft tissues lose flexibility, and healing fibres may settle in a shortened pattern instead of aligning along normal movement lines. If, on the other hand, you repeatedly push into the same deep, painful bends and twists, you keep tugging on healing tissue and can keep irritation going. Most people do best with a middle‑ground approach: gentle movement in a comfortable middle part of your movement, and gradual return to fuller movement and lifting as pain allows.
What usually helps this kind of back pain settle
For a straightforward strain or sprain, it often helps to:
- keep moving little and often, within a range that feels safe, rather than staying completely still,
- use small walks and simple changes of position to ease stiffness without overstressing the injured area,
- as pain allows, gradually bring back deeper bending and lifting, using better technique — hips back, knees slightly bent, back fairly straight instead of fully rounded, and loads held closer to your body,
- spread heavier jobs through the day instead of doing them all at once.
These steps support healing and reduce the chance of the same tissues being repeatedly overloaded as they repair. Once the worst of the acute episode has settled, the broader approaches described earlier on the main page for posture‑linked back pain also apply here and can reduce the risk of repeated strains in the same area.
How this brace can help in back strains and sprains
In the early phase of a strain or sprain, the main mechanical problems are pain and spasm when healing fibres are stretched too far or too fast, and a sense that one wrong move will “set it off” again. A brace can help if it:
- limits your very deepest bends, arches and twists, so healing fibres are less likely to be pulled sharply,
- provides gentle, even compression so movement feels more contained and supported,
- reminds you to stay within a safer middle band of movement while tissues heal.
The BackReviver Posture Support Back Brace does this through its semi‑rigid stays, which resist sharp forward bends and sudden twisting, and its belt and pad, which give a steady hold around the lower back. As you begin to move towards angles that have been provoking, you feel the brace offer resistance, prompting you to adjust and reducing the chance of a sudden, painful tug on the injured area. By reducing these sudden stretches, it can also help calm reflex muscle spasm.
Using the brace if you have a back strain or sprain
If you are dealing with a recent strain or sprain:
- use the brace around the activities that most often hurt — such as preparing meals, light tidying or standing conversations — rather than wearing it from morning to night,
- tighten it so the back feels supported and a little more secure, but not so far that you feel squeezed or short of breath,
- take it off or loosen it fully when you are resting, lying down or doing very gentle movements.
As pain eases and you gain confidence, shorten the periods you use the brace so your own muscles gradually take over more of the work again. For many people, the brace is most useful in the first few days to weeks after a strain, during more demanding moments of the day, rather than as something to rely on long‑term. If pain remains very strong, spreads into the legs, or is not improving after a couple of weeks, arrange a review with a clinician to rule out other causes and plan further rehabilitation.
For Mixed Mechanical / Non‑specific Low‑Back Pain
Does this sound like your back pain?
This overview is for you if someone has described your back pain as “mechanical” or “non‑specific”, or if you recognise a mix of:
- ache or stiffness across the lower back that builds with long sitting or standing and eases when you move,
- sharper twinges with certain bends or twists, especially when you are tired,
- flare‑ups after days with more bending, carrying or driving than usual.
If you recognise most of these features, your back pain is likely to be driven more by how your spine is loaded and moved over the day than by a single specific injury.
What is usually going on in your back
In this kind of back pain, several structures often become sensitive at the same time:
- Discs may be less springy and more sensitive to prolonged slumped positions or repeated deep bending.
- Facet joints may feel overloaded when you lean back or twist sharply, especially if discs have lost some height.
- Ligaments and joint capsules can complain when you regularly push into your deepest bends and arches.
- Muscles may be doing too much holding in some postures and not enough strengthening work overall, leading to fatigue, tightness and guarding.
Back pain tends to develop when these tissues are repeatedly stressed in ways they do not tolerate well, and when the muscles that should be sharing the load are not doing enough of it.
Who tends to get this kind of back pain
This type of mechanical back pain is very common in adults, particularly in those who:
- spend many hours most days sitting without regular breaks,
- do repetitive bending and twisting at work or at home,
- are in mid‑life and beyond with age‑related disc and joint changes,
- have had previous episodes of back pain and resumed full activity quickly without rebuilding strength and control.
Many adults develop this kind of back pain gradually over time, so if this sounds familiar, you are not unusual.
Why it can drag on if nothing changes
Non‑specific mechanical back pain can limit what you feel able to do at work and at home. It may make it harder to sit through the working day, manage household chores, or keep up with family and hobbies.
Pain often becomes more persistent when:
- you keep exposing your back to the same aggravating postures and loads without changing anything,
- fear of pain leads you to guard and move less so that muscles weaken further,
- each flare is treated as something separate rather than part of a wider pattern linked to how you sit, stand and move over time.
Over time, this can turn what began as occasional “bad days” into a background problem that flares more easily and takes longer to settle.
What usually helps this kind of back pain settle
Most people with this kind of pain do better when they:
- stay as active as they reasonably can within their limits, rather than resting completely whenever pain appears,
- sit and stand in a more comfortable middle posture — not heavily slumped and not heavily arched,
- break up long periods in one position with brief changes of posture or short walks,
- bend and lift with safer mechanics where possible,
- work on strength and coordination in the deep muscles around the spine and hips with exercises chosen for them.
Adjusting work and home set‑ups so that better postures are easier to achieve often makes a real difference. The general approaches described earlier on the main page for posture‑linked back pain — keeping moving, adjusting set‑ups and gradually strengthening the trunk and hips — are particularly important here, because several structures are sharing the load of your pain.
How this brace can help if you have mixed mechanical low‑back pain
When your back pain is non‑specific and mechanical, this brace is not targeting one single disc or joint. Its role is to help you spend less time in the positions and extremes of movement that you already know tend to set your pain off. In practical terms, that means helping you:
- hold a more comfortable, upright posture when you would otherwise slump or over‑arch,
- move less often into your very deepest forward bends and backward leans, especially when you are tired or not paying attention,
- feel that your lower and mid‑back are held more steadily, so small, sharp movements at a single sore level are less likely.
The BackReviver Posture Support Back Brace does this through its full‑length back panel, which prompts you when you start to round forwards or lean back too far, and its firm lumbar belt and pad, which support the lower levels and resist sudden, large changes in angle. By reducing repeated deep slumps and arches and sudden, uncontrolled movements, it can lessen strain on the outer rings of your discs, your facet joints and the ligaments and capsules around them, and reduce the amount of “guarding” work your muscles feel they have to do.
Using the brace if your pain is called “mechanical” or “non‑specific”
If your pain has been described in these terms:
- think about when it typically builds: after a long stretch at a desk, long periods on your feet, a certain type of housework, or a particular leisure activity such as a long walk or a hobby that involves leaning forwards,
- use the brace for those tasks, tightening it so that your back feels clearly supported but you can still move and breathe easily,
- take it off or loosen it between those blocks so your muscles continue to work,
- use the extra comfort and security to help you keep moving and to work through your exercise and posture plan, rather than to avoid movement.
If your back pain feels very different from what you are used to, spreads in an unusual way, or is not improving with these steps, arrange a further assessment.
For Degenerative Disc Disease
What disc‑related low‑back pain usually feels like
Degenerative disc disease describes age‑related changes in a disc where it dries out, loses some height and may develop small tears in its outer ring. Many people have such changes on scans and never have pain. When a degenerating disc is part of the pain picture, a familiar pattern is:
- a deep, central ache across the lower back that builds with long sitting — especially in a slumped posture or on very soft seating,
- stiffness and pain when standing up from a chair after a long drive or meeting, with some easing as you walk,
- ache or sharpness with repeated forward bending, such as loading a dishwasher, picking things from the floor or working at a low surface.
Some people also describe a sense of deep “tiredness” or “pressure” in the lower back after long sitting, rather than a sharp surface pain.
What is happening in the disc and nearby tissues
A healthy disc has a water‑rich, gel‑like centre and a tough outer ring of fibres. With age and repeated loading:
- the centre can lose water and become less springy,
- small splits can appear in the outer ring,
- the disc loses some height and may bulge a little,
- the bony endplates above and below the disc can become sensitive.
When disc height is reduced, the vertebral bodies sit closer together, the outer ring and endplates take more load, the way the facet joints and ligaments share load changes, and the vertebrae can tilt and slide slightly more on one another, especially when you bend deeply or sit slumped for long periods. These small extra tilts and slides, and the increased strain on the back‑outer disc ring and endplates, can be painful when the tissue is irritable. That is why repeated deep slumps or heavy forward bends tend to bring on or “wind up” this kind of pain, especially when you are already tired or have been sitting for a long time.
Who tends to develop painful disc degeneration
Disc degeneration is very common as people get older. Many adults have degenerative discs visible on X‑ray or MRI, whether or not they have symptoms. Pain is more likely if:
- several discs have lost height and flexibility,
- you spend long periods in slumped sitting or repeated deep bending,
- supporting muscles are relatively weak so discs and joints take more of the day‑to‑day strain,
- you have had previous disc problems and returned to high loads without gradually rebuilding support.
Scan findings on their own do not prove that a disc is causing your pain. What matters is how your back behaves and how different positions and movements affect your symptoms.
Why disc‑related pain can become long‑term
Disc changes themselves do not reverse, but the way the spine behaves can be influenced. Pain can persist when:
- you repeatedly load the disc in its most troublesome positions — deep slumps and heavy bending — without changing anything,
- pain leads you to avoid bending altogether so that muscles weaken and joints stiffen,
- the endplates and outer disc fibres are repeatedly stressed and not given enough time in more comfortable postures to settle.
Simply resting does not teach the disc and surrounding structures to cope better with load; pushing on into the same painful positions without building strength and control tends to keep irritation going. Most people do best with a middle‑ground approach: regular movement, targeted strength work and task planning and set‑up changes that keep the disc within a level of strain it can manage more of the time.
What usually helps this kind of disc pain settle
If a degenerating disc is part of your problem, it often helps to:
- sit with your lower back supported in a gentle curve rather than heavily slumped, especially for longer spells,
- break up long sitting and driving with brief standing or walking,
- bend by using your hips and knees and keeping your lower back in a comfortable middle posture, rather than rounding deeply from the waist,
- bring work up closer to around waist height where possible,
- strengthen the deep muscles supporting your lower back and the muscles around your hips, using exercises chosen for you.
These steps reduce repeated high strain on the back‑outer part of the disc and endplates and help the surrounding muscles and joints support the area better. The general approaches described earlier on the main page for posture‑linked back pain — staying active, adjusting postures and strengthening — are especially relevant here.
How this brace can help if you have degenerative disc disease
In painful disc degeneration, the main mechanical irritants are:
- increased pressure and strain on the back‑outer part of the disc and nearby ligaments during deep slumps and heavy bending,
- small extra sliding movements between vertebrae at the affected levels.
A posture support brace can help if it:
- encourages a gentle, natural curve in the lower back instead of a full slump,
- helps your trunk behave a little more as a unit so sudden shear at the painful level is reduced,
- helps you notice when you are moving into the deeper bends that usually set your pain off.
The BackReviver Posture Support Back Brace does this through its lower‑back pad and semi‑rigid stays, which support the lumbar spine in a more neutral curve and resist deep forward bending, and its even belt, which adds light compression and reduces small, uncontrolled sliding at the affected level. The full‑length panel helps you notice when you are starting to sag forwards, prompting earlier correction. By doing this, the brace reduces repeated high stress on the sensitive outer ring of the disc and the endplates, which are often the source of pain in this kind of problem.
Using the brace if your disc is part of the problem
If disc changes have been identified as part of your back pain, or your pattern strongly fits disc‑related pain:
- think about when your disc‑related pain tends to worsen — long sitting, long drives, or periods of repeated forward reaching,
- use the brace for those activities to help you maintain a more comfortable posture and avoid your deepest slumps and bends,
- adjust the belt so that your lower back feels clearly supported but you can still breathe and move reasonably freely,
- take breaks without the brace so your muscles continue to work, and use the comfort and control it gives to help you work on your strengthening and movement programme,
- as your back copes better with sitting and bending, shorten the time you rely on the brace and keep it for more demanding days or flare‑ups.
If your pain pattern changes significantly, spreads, or no longer clearly links to posture and movement, arrange a review with a clinician to check that disc‑related irritation is still the main driver and that this level of support is still appropriate for you.
For Spondylosis (Facet‑Predominant Osteoarthritis)
What facet‑predominant spondylosis often feels like
Spondylosis is a term for age‑related wear in the spine. When the small joints at the back (facet joints) are a major part of the problem, people often report:
- a dull ache and stiffness across the lower back after sitting or standing for a while,
- stiffness first thing in the morning that improves as they move,
- sharper pain if they lean backwards or twist quickly,
- ache spreading into the buttocks or the back of the thighs.
You may feel “rusty” at the start of the day, ease as you get going, then feel pain return after long standing or repeated twisting and leaning back.
What is happening in the joints and discs
Over many years, discs gradually lose some water and height. As that happens:
- more of the load is carried by the facet joints,
- the cartilage on their joint surfaces can thin,
- the joint capsules and surrounding ligaments can thicken,
- small bony spurs can form.
These changes are very common in middle‑aged and older adults and are often seen on imaging. They do not always hurt. When they do, it is usually because:
- leaning back (extension) closes down and compresses the facet joints, squeezing irritated joint surfaces and capsules,
- sharp twisting loads the joints unevenly,
- prolonged slumped sitting strains the back‑outer part of the discs and ligaments, which may already be sensitive.
The combination of joint wear, altered disc height and repeated extension and twisting can make the lower back stiff and sore.
Who tends to develop this kind of back pain
Facet‑predominant spondylosis is common in adults in mid‑life and beyond, especially in those who:
- have spent many years in manual work, repetitive lifting or driving,
- stand a lot without much movement,
- have had earlier disc problems or spinal injuries,
- have reduced general strength and fitness.
Many people with spondylotic changes on scans will not have symptoms; in those who do, the changes and certain movement habits combine to create the ache and stiffness described.
Why facet‑related pain can persist
Spondylosis can reduce how long you can stand or walk comfortably, make deep backward leans and quick twists feel painful, and shrink the range of motion that feels safe and comfortable in the lower back.
Pain tends to persist when:
- you continue to spend a lot of time in the positions that squeeze the facet joints hard — deep arches and prolonged static standing — without adjusting them,
- you respond to pain by moving less so supporting muscles weaken and joints stiffen,
- underlying strength, flexibility and posture issues are not addressed.
If pain continues to get worse, stiffness becomes very limiting, or leg symptoms such as numbness, weakness or tingling develop, or if bladder or bowel control changes, an assessment is needed to check for nerve involvement or other causes.
Practical changes that often help this kind of back pain
Many people with this back‑joint problem find they cope better when they:
- keep the lower back in a comfortable middle posture — not heavily slumped and not heavily arched — especially when standing,
- turn by moving their feet and hips together rather than twisting sharply at the waist,
- break up longer periods of standing or walking with short rests,
- carry loads closer to the body and avoid twisting under load,
- build trunk and hip strength and general fitness with a suitable exercise plan.
These steps reduce time spent in the positions that squeeze facet joints hard or strain the back of the discs and ligaments. In simple terms, you are trying to spend less time leaning back on stiff, worn joints and more time in the middle of your movement where those joints are under less pressure. The more general activity and strengthening steps described earlier on the main page also support this.
How this brace can help if you have spondylosis
In facet‑predominant spondylosis, the aggravating movements tend to be deep backward bending, which compresses the facet joints; sharp twisting, which loads them unevenly; and prolonged slumping, which strains the back of the discs and ligaments. A brace can help if it gently limits how often and how far you lean back and twist, and supports a moderate curve in the lower back so heavy slumps are less likely.
The BackReviver Posture Support Back Brace helps in this way by:
- using semi‑rigid stays in the lumbar belt to resist deep extension and sudden twists,
- using its belt and pad to support a comfortable lumbar posture rather than a deep arch or collapse.
Together, these features reduce repeated facet compression and strain on the capsules and ligaments around them, as well as reducing repeated stress on the back‑outer parts of the discs. That can make standing, gentle turning and ordinary bending feel less likely to provoke symptoms.
Using the brace if you have spondylosis
If your back pain has been linked to spondylosis:
- consider using the brace for tasks and times when you tend to lean back, twist quickly or stand in one spot for a long time — for example, particular work roles, periods of queueing, or household jobs involving looking or reaching behind you,
- position the brace so the lower‑back pad supports the area that usually aches and adjust the belt evenly until you feel a firm but comfortable hold,
- loosen or remove it for sitting and quieter periods and keep exercising and moving without the brace so your muscles stay active.
If symptoms escalate or nerve‑type features appear despite these steps, arrange further assessment rather than trying to manage the change by altering how you use the brace.
For Sacroiliac Joint Dysfunction
What sacroiliac joint pain usually feels like
The sacroiliac joints (SIJs) sit where the base of your spine (sacrum) meets the pelvic bones on each side. When they are painful, you often feel:
- a deep ache or sharp pain over one buttock, near the small “dimples”,
- pain spreading into the side of the hip or down the back or side of the thigh, usually stopping above the knee,
- worse pain with one‑leg tasks — standing on one leg to dress, going up stairs, walking uphill, turning in bed,
- easier symptoms when you share weight evenly between both legs or buttocks.
You might notice that longer walks, particularly on uneven ground or hills, and repeated twisting or stepping across the midline tend to provoke symptoms.
What is happening in the joints
The sacroiliac joints are strong, wedge‑shaped joints with interlocking bony surfaces and strong ligaments. They normally move only a little. With each step and turn, there is a small amount of sliding and tilting between the sacrum and pelvis.
Pain can develop when:
- ligaments or joint capsules have been strained — for example after a fall or awkward lift,
- pregnancy‑related hormonal changes and altered load increase joint mobility and sensitivity,
- repeatedly loading one side more than the other, or leg‑length differences, increase small sliding movements (shear forces) across the joints.
Once the joints or supporting ligaments are irritable, even these small shears can feel painful, especially in single‑leg positions and quick turns.
Who tends to develop sacroiliac joint problems
Sacroiliac joint pain is less common than general lower‑back pain but is seen regularly. It is more likely:
- after pregnancy, when ligaments have been naturally more stretchable and the way weight is carried has changed,
- in people with leg‑length differences or marked foot/hip alignment issues,
- in those who regularly carry heavy loads on one side or often stand on one leg,
- after falls onto the buttocks or lower back.
It may occur on its own, or alongside other lower‑back problems.
How it affects everyday movement and why it can drag on
SIJ pain can make walking, using stairs and turning in bed uncomfortable and awkward. Standing on one leg to put on trousers or shoes often provokes symptoms. Longer walks, particularly on slopes or uneven ground, can bring on ache and fatigue around the pelvis. You might notice that you start to plan around these moments — for example, sitting down to dress instead of standing on one leg, or avoiding certain routes because you know the hills or uneven ground will set things off.
If you respond by avoiding using the painful side or stiffening your trunk, you may start to load the other side more, move less fluidly, and strain muscles and joints elsewhere. That can prolong the problem and spread discomfort beyond the original area.
What usually helps this kind of sacroiliac pain settle
Helpful measures often include:
- standing and sitting with weight spread more evenly between both sides, instead of leaning on one hip or perching on one buttock,
- taking slightly shorter steps on hills and stairs to reduce sliding forces across the joints on each stride,
- learning to roll in bed by moving shoulders and hips together rather than twisting the lower trunk and pelvis separately,
- splitting one heavy load into two lighter ones and holding them closer to your body,
- working on strength and control in the muscles around your hips and the deep muscles of your abdomen so the pelvis moves more steadily.
All of these aim to reduce quick, uneven sliding at the joints and to support smoother movement of the trunk over the pelvis. In practical terms, this means your pelvis moves more steadily under you, rather than one side taking most of the strain. The more general activity and strengthening principles described earlier on the main page also apply.
How this brace can help if you have sacroiliac joint pain
In sacroiliac joint dysfunction, the key mechanical problems are excessive or poorly controlled sliding between the sacrum and pelvic bones, and small, poorly controlled shifts of your upper body over your pelvis, especially when you are on one leg. A brace can help if it:
- encourages the lower trunk and pelvis to move more as a single, steady unit,
- reduces sudden shear forces across the joints,
- supports more even weight‑bearing.
The BackReviver Posture Support Back Brace does this by:
- wrapping around the lower back and upper pelvis with a broad belt and pad, helping the sacrum and iliac bones move together rather than sliding too much against each other,
- using flexible stays to provide gentle control from above, limiting sudden twisting of the trunk that would otherwise be transmitted down to the sacroiliac joints.
That combination can make walking, using stairs and other activities that involve a lot of stepping feel more steady and less provocative, and can reduce strain on the ligaments that hold the joints together.
Using the brace if you have sacroiliac joint dysfunction
If your pain has been traced to the sacroiliac joints:
- fit the brace so the belt and pad support the lower back and upper pelvic region,
- tighten it from both sides until your lower trunk feels more stable but not squeezed or uncomfortable,
- use it for activities that consistently bring on SIJ symptoms — such as longer walks, stair use, shopping or particular housework — and loosen or remove it for rests and lower‑load tasks.
If you have a separate low pelvic belt prescribed by a clinician, wear that first, then this brace over the top to add trunk support, if advised. Keep working on even weight‑bearing, stride length and strengthening work as recommended. If pain remains unchanged or spreads despite these measures, ask for further assessment rather than simply relying more heavily on the brace.
For Lumbar Segmental Instability (Micro‑instability)
What lumbar “instability” usually feels like
Here, “lumbar segmental instability” means that one or two levels in the lower back are moving a bit more, or less smoothly, than they should — not that the spine is about to give way completely.
People often describe:
- a background ache when they sit or stand in one position for a while,
- stiffness or “rustiness” when first standing up, easing a little with gentle walking,
- sudden catches or sharp twinges at specific angles, especially with combined bending and twisting,
- a sense that the back feels “better when supported”.
You may recognise the feeling of your back “snatching” or “grabbing” momentarily when you move through certain parts of a bend or twist.
What is happening between the vertebrae
Each level in the spine consists of two vertebrae, the disc between them at the front, a pair of facet joints at the back, and the ligaments and muscles around them. Normally:
- the disc, ligaments and joint capsules provide restraint and limit how far the bones can slide or tilt,
- the small deep muscles provide active control and help guide movement.
In segmental instability at one level:
- the ligaments, disc and joint capsules at that level may be a little lax or irritated,
- the local muscle control at that level may not be working as well as it should at certain angles.
As you move into or out of particular positions, that level can then move slightly more, or less smoothly, than the others. These small extra or poorly controlled movements stress the outer ring of the disc, ligaments and joint capsules, which is why catches or twinges occur at specific points. In this context, “instability” is about these small control problems, not the spine slipping out of place completely.
Who tends to develop this kind of problem
This situation is seen reasonably often in adults who:
- have had repeated minor back strains or sprains at a similar level,
- switch between periods of very little activity and heavier tasks without building up gradually,
- sit for long periods with relatively weak trunk muscles,
- have had surgery or injury that altered the passive support around one level.
It may not always be labelled “instability” in consultations, but comments such as “it catches at a certain point” or “it feels better when something supports it” are common.
How it affects movement and confidence
Segmental control problems can make everyday tasks feel risky. Bending to pick up objects, gardening, tidying low shelves or lifting and turning can all bring on catches or sharp twinges at particular angles. Getting out of a low chair or car seat may involve a “sticky point” where you brace for a possible jab of pain.
In response, you may start to move more stiffly and brace your back constantly, or avoid certain movements altogether. That reduces the chance for the deep stabilising muscles to work and can reinforce a cycle where pain leads to avoidance, avoidance leads to poorer control and poorer control leads to more pain and catching.
Why it helps to tackle control, not just pain
The looseness in some of the supporting ligaments and joints at that level may not disappear, but active control from muscles and the nervous system usually can improve. Targeted work on the strength and timing of the deep trunk and hip muscles, along with graded re‑introduction of previously feared movements, can reduce catching, improve confidence and lower day‑to‑day ache.
This often includes low‑load control exercises in lying or on hands and knees that train the deep stabilising muscles to work more reliably. Relying only on rest, intermittent supports or passive treatments, without building control, is less likely to lead to lasting change.
How this brace can help if you have segmental instability
In this situation, the main mechanical issues are small, poorly controlled movements at particular levels when you move into and out of certain positions, and sudden changes in angle at those levels when you bend, arch or twist deeply. A brace can help if it:
- provides a little extra support around your trunk so the spine moves more as a controlled unit,
- encourages you to stay in the comfortable middle part of your movement instead of pushing into your deepest bends and arches,
- reduces the chance of sharp, isolated movements at the sensitised level.
The BackReviver Posture Support Back Brace helps by using its lower‑back pad and belt to hold the lumbar region evenly, making sudden, sharp changes in angle at one level less likely, and its semi‑rigid stays to resist deep forward bending and sudden twisting. The full‑length panel supports a straighter overall posture, which reduces uneven loading between levels. In practice, that often feels like fewer sharp catches in the same spots when you bend or twist.
Using the brace if your back “catches”
If your back pain includes catching or twinges at certain angles:
- use the brace around the activities where this happens most — such as longer sitting periods, repeated reaching or short bouts of lifting and carrying,
- tighten it so your lower back feels more secure and you are gently discouraged from deep bending and twisting, but you can still move reasonably freely,
- remove or loosen it for quieter times and when you are doing exercises designed to improve control, so your muscles get the chance to strengthen,
- as your strength, timing and confidence improve, aim to use the brace less often and keep it for the most demanding days or tasks.
If catches become more frequent or severe, or new leg symptoms such as numbness, weakness or changes in bladder or bowel control develop, seek further assessment rather than simply tightening the brace.
For Spondylolysis (Pars Stress Injury, No Slip)
What a pars stress injury tends to feel like
Spondylolysis is a stress injury or small defect in a narrow bridge of bone at the back of a vertebra called the pars interarticularis. It most often affects the lowest lumbar vertebra.
People with this problem often report:
- lower‑back pain that is clearly worsened by leaning backwards,
- pain with sports or jobs that repeatedly arch and twist the lower back,
- some relief with rest or by leaning slightly forwards,
- tight hamstrings and a slightly shortened stride when walking.
Pain may be sharper during or after activities that repeatedly demand extension and rotation of the lower back, and may ease between flare‑ups.
What is happening in the pars
The pars interarticularis is a small bridge of bone that connects the upper and lower parts of the vertebral arch and helps support the facet joints. It also helps resist forward slip of the vertebra.
In activities and sports with repeated back‑bending and twisting — such as some gymnastics‑type movements, fast bowling actions, some martial arts or acrobatic activities, and certain manual tasks — this narrow bony bridge is repeatedly stressed.
Over time, this can cause:
- a stress reaction in the pars, where bone turnover increases and the area becomes painful,
- a small crack or defect if loading continues unchanged.
A painful pars is sensitive to extension and rotation. If a complete defect develops on both sides and is left unaddressed, it can make a forward slip more likely later on, although that does not happen in every case.
Who tends to develop spondylolysis
Pars stress injuries are less common than general back pain, but they are regularly seen in:
- people who take part in sports or activities with repeated back‑bending and twisting,
- adults who developed a pars injury earlier in life and have continued with similar physical demands,
- some workers who frequently arch and twist the lower back under load.
If this describes your experience, your lower back has likely been working against extension forces for many years before this pain became more obvious.
How it affects movement and sport or work
Spondylolysis can:
- limit participation in sports that demand repeated back‑bending and twisting,
- reduce tolerance for standing for long periods with an arched posture,
- cause pain with overhead tasks or reaching backwards.
If not recognised and managed, continuing the same extension‑heavy activities tends to keep the pars irritated, slow or prevent healing and, in some cases, contribute to a slip at that level.
Why early and structured management helps
When a pars injury is suspected or confirmed, the usual aims are to:
- reduce the specific extension and rotation loads that caused the problem,
- allow bone healing or settling,
- keep the rest of the body as conditioned as is reasonable,
- plan a graded return to training or manual work.
That usually involves reducing or modifying extension‑heavy activities for a period, often under specialist guidance, and using a structured exercise plan to maintain and then rebuild strength and control in the trunk and hips. Continuing full, unmodified activity often slows recovery; stopping almost all movement with no plan can create new problems.
How this brace can help if you have spondylolysis
For a pars stress injury, the main mechanical irritants are backward bending at the lumbar spine and quick twisting movements. A brace can help if it:
- limits how far and how often you extend the lower back in day‑to‑day standing and light activity,
- reduces sudden twists,
- encourages a more neutral lumbar posture outside of specific training or treatment sessions.
The BackReviver Posture Support Back Brace is designed to:
- use semi‑rigid stays in the lower belt to resist extension and twisting, which lowers repeated stress through the pars during normal walking, standing and light tasks,
- provide an even hold around the waist so the lower back moves more as one controlled unit, rather than hinging repeatedly at the painful level,
- give gentle feedback through the back panel and straps when you start to lean back more than usual, reminding you to ease off before you reach the positions that usually hurt.
Reducing repeated stress on the pars in this way gives the bone a better chance to settle or heal as part of the wider treatment plan set out by your clinician.
Using the brace alongside your pars injury plan
If a pars injury has been identified:
- use the brace for daily standing, walking and lighter tasks where you tend to drift into a deep arch or feel unprotected — for example at work, travelling, or doing housework,
- tighten it to a firm but comfortable level that clearly discourages you from arching your lower back, but does not stop you breathing or moving normally,
- follow your clinician’s advice on how far to reduce extension‑heavy sports or work and when to start building them back in,
- do not treat the brace as permission to carry on with unmodified heavy back‑bending and twisting; it is there to support the reduction and gradual re‑build plan you have been given.
As pain settles and your back’s tolerance improves under guidance, gradually reduce general brace wear so that, in the long run, control comes from your own strength and technique rather than from external support.
For Spondylolisthesis
What spondylolisthesis can feel like
Spondylolisthesis means one vertebra has slipped forwards slightly on the one below. In adults, this usually affects the lower lumbar spine. Not everyone with a slip has symptoms. When it does cause problems, people often notice:
- lower‑back or buttock pain that worsens when they stand for longer periods,
- a feeling of compression or discomfort when leaning back (for example reaching overhead or “standing very upright”),
- easier symptoms when they sit or lean forwards a little,
- aching, heaviness or tingling in the buttocks or legs during longer walks, especially when going downhill or walking on level ground for some distance.
You may find you need to stop, sit, or lean forwards over a support after walking for a certain distance.
What is happening at the slipped level
Broadly, there are two common types in adults:
- Degenerative spondylolisthesis: discs lose height and facet joints wear, so alignment and load‑sharing change and the upper vertebra slides forwards slightly.
- Isthmic spondylolisthesis: a defect in the pars interarticularis (often from an old stress injury) weakens the back of the vertebra and allows more slip.
At the slipped level:
- the front of the upper vertebra sits further forwards,
- the facet joints and ligaments behind are under altered tension,
- leaning backwards increases forward‑sliding forces,
- extension narrows the openings where nerve roots leave the spine (foramina), which can irritate or compress them and contribute to leg symptoms.
Deep slumping and flexion can still stress the disc, especially if it is already degenerated, but for many people with a symptomatic slip, prolonged upright standing and back‑bending are more problematic than gentle forward‑leaning.
Who tends to develop spondylolisthesis
Spondylolisthesis is relatively common on imaging in:
- older adults with degenerative spinal changes,
- adults who had pars defects from extension‑heavy sports earlier in life.
Many people have small slips found incidentally on imaging and never develop symptoms. Pain and functional problems are more likely when:
- the slip is moderate or accompanied by significant disc and facet‑joint wear,
- postures and activities involve frequent back‑bending and prolonged upright standing,
- trunk and hip muscles are relatively weak and balance is reduced.
How it affects movement and why it matters
A symptomatic slip can:
- limit how long you can stand without back or leg symptoms,
- make overhead reaching and standing with the hips pushed forwards and chest lifted uncomfortable,
- reduce confidence when walking on slopes or uneven ground.
If the slipped level and nearby structures narrow nerve spaces significantly, you may experience leg pain, numbness, weakness or heaviness with walking or standing (sometimes called neurogenic claudication), and relief when leaning forwards — for example resting on a trolley handle or leaning on a work surface. Ignoring increasing pain, dropping walking distances, or new leg symptoms is unwise; these changes should be assessed and managed appropriately.
Practical changes that often help this kind of back pain
Many people with spondylolisthesis do better when they:
- keep their lower back in a fairly straight, comfortable posture and avoid deep arches during standing,
- bring overhead tasks down and closer so they do not have to lean back to reach,
- use slight forward‑leaning positions such as resting the hands on a trolley handle for longer walks if these ease symptoms,
- break up prolonged standing with short sitting or forward‑leaning rests,
- work on hip and trunk strength and controlled movement under guidance.
These steps reduce time spent in positions that increase forward sliding and close down nerve spaces. The more general activity and strengthening steps described elsewhere on the main page also apply.
How this brace can help if you have spondylolisthesis
In a slip that is causing symptoms, the mechanical problems are increased forward sliding and joint irritation when you bend backwards, narrowing of foramina and possible nerve irritation with extension, and a tendency to stand in more extended postures, especially when tired. A brace can help if it:
- limits how far and how often you lean back,
- supports a straighter lumbar posture for standing and reaching,
- reduces time spent in extension‑heavy positions.
The BackReviver Posture Support Back Brace does this by:
- using semi‑rigid stays in the lumbar belt to resist deep extension, reducing extra forward sliding and continuous facet compression at the slipped level,
- using the belt and pad to support the lower back evenly so you are encouraged to stand more neutrally instead of with your hips pushed forwards and back heavily arched,
- using the full‑length panel to help you notice when you are starting to lean back too far and prompting earlier adjustment.
By reducing repeated deep backward leans, the brace also helps reduce how often the openings for the nerve roots are narrowed as much. It does not reverse the slip, but it can make standing and walking feel more controlled and less likely to provoke symptoms while you work on strength and posture.
Using the brace if you have a slip
If you have been told you have a symptomatic slip:
- use the brace during activities that typically involve prolonged standing or repeated leaning back — such as particular work tasks, queueing, social events on your feet, or overhead jobs,
- fit it so the pad supports the lower back over the region that usually hurts,
- tighten the belt evenly until you feel well supported and less tempted to lean backwards, but can still move and breathe comfortably,
- loosen or remove it when you sit, lean forwards to rest or carry out your exercises.
Combine brace use with strengthening, posture training and activity‑planning as recommended. If your walking distance is falling, leg symptoms are worsening, or you develop changes in bladder, bowel or saddle‑area sensation, seek medical advice promptly; a brace alone is not enough in the face of progressive nerve compromise.
For Back‑related Leg Pain (Sciatica‑type Patterns)
What back‑related leg pain can feel like
People often use the word “sciatica” to describe leg pain linked to a back problem. By sciatica, most people mean:
- pain starting in the lower back or buttock and travelling down the back or side of the thigh, sometimes towards the calf or foot,
- tingling, numbness or “pins and needles” in part of the leg,
- a feeling of heaviness or weakness in the leg, particularly after walking or standing.
You might notice that certain back positions make the leg worse — for example, a deep slump or a strong lean back — and that other positions ease it. Leg pain that changes with back position is understandably worrying, and it is important to have it assessed properly.
What is happening in the nerves and spine
Back‑related leg pain often involves irritation or compression of a nerve root where it leaves the spine. This can happen when:
- a disc bulges or herniates and presses on or irritates the nerve root,
- the opening where the nerve root exits (foramen) narrows due to bony changes, disc height loss or thickened ligaments,
- a slipped vertebra (spondylolisthesis) or marked wear changes alter alignment and space around the nerve.
Different nerve roots supply different areas of the leg. For example, irritation of the L5 nerve root often causes pain or tingling down the outer calf and into the top of the foot, while irritation of the S1 nerve root can cause symptoms down the back of the calf and into the sole or outer side of the foot.
Deep slumped sitting and repeated heavy bending can increase pressure on the back‑outer part of the disc and on the nerve root in some people. Standing very upright or leaning backwards can narrow the foramina and irritate nerve roots in other situations, especially when these movements are held for some time.
When leg pain needs urgent or quick assessment
Some symptoms suggest that nerves in the lower spine may be under significant pressure. This can sometimes be due to conditions such as a large disc prolapse or severe narrowing in the spinal canal (cauda equina syndrome). These situations are uncommon, but they need urgent assessment because delayed treatment can increase the risk of permanent nerve damage.
Seek same‑day urgent medical assessment — for example at an emergency department or urgent assessment service — if you notice:
- new difficulty controlling your bladder or bowels, or not realising when you need to go,
- numbness or loss of feeling in the groin or inner buttocks (the “saddle” area),
- rapidly worsening weakness in one or both legs, or difficulty lifting the foot when walking,
- severe back pain after a fall, crash or other significant injury, especially if you also notice leg symptoms.
These symptoms are not things to manage yourself with a brace; they need urgent medical assessment. You should also arrange prompt assessment if leg pain is severe and persistent, numbness or tingling is spreading, your walking distance is dropping quickly because of leg symptoms, or you have unexplained weight loss, fever, or a history of cancer with new back or leg pain. The safety section on the main page explains these warning signs in more detail.
How back position can influence leg symptoms
For some back‑related leg problems, certain postures are clearly better or worse. For example:
- In some disc‑related problems, deep slumped sitting and repeated heavy bending can increase pressure on irritated disc tissue and the nerve root, worsening leg pain. Standing upright or walking gently may ease it.
- In some slip‑related or narrowing (stenosis) cases, standing very upright or leaning backwards can worsen leg symptoms by narrowing the foramina where nerves exit, particularly during longer walks or when standing still. Slight forward‑leaning positions — such as resting your hands on a trolley handle while walking — often bring some relief.
These responses vary between people, which is why, if you have sciatica‑type symptoms, they should be assessed and you should be given specific guidance on which positions and movements are better and worse for your case.
Where a brace may fit in (and where it does not)
This brace cannot diagnose or fix nerve problems on its own, and it is not a cure for sciatica. Many people with back‑related leg pain need a combination of information, exercise, medicines and sometimes procedures or surgery, depending on the underlying cause.
In some back‑related leg‑pain cases, once a clinician has checked that a lumbar support is safe and appropriate for you, a brace may have a limited role. It can help by making it easier to avoid the spinal positions that clearly aggravate your leg symptoms. For example:
- In some slip‑related or narrowing patterns, it can reduce deep backward bending and help you hold a straighter posture in standing so the foramina are not repeatedly closed down.
- In some disc‑related patterns, it can reduce repeated deep slumped sitting, which may lower pressure on irritated disc tissue and the nerve root.
By encouraging you to stay closer to the postures your clinician has identified as less likely to aggravate the nerve, the brace can contribute to symptom management. It should always be used alongside, not instead of, assessment and rehabilitation, and only within the guidance you have been given.
Using the brace if you have back‑related leg pain (with clinical advice)
If you have sciatica‑type leg pain and a clinician has said this kind of brace is suitable for you as part of your plan:
- follow their advice on which postures and movements tend to help or worsen your leg symptoms,
- wear the brace at times when you tend to slip into the “worse” positions — for example, prolonged upright standing with backward lean in some slip‑related patterns, or long, slumped sitting in some disc‑related patterns,
- adjust the belt so you feel supported and gently steered away from those positions without feeling restricted in breathing or completely stiff,
- do not use the brace to push into movements you have been told to avoid,
- continue with any exercises and activity‑planning strategies you have been given.
If your leg symptoms change significantly — for example, worsening pain, spreading numbness or new weakness — arrange a further assessment rather than simply altering how you wear the brace.
For Kyphosis
What kyphosis‑related back pain usually feels like
Kyphosis describes an increased forward curve in the upper or mid‑back. In many older adults a gentle curve is normal; in some people it becomes more pronounced. When this curve is part of your pain, you may notice:
- a visible rounded upper‑back posture, sometimes with the head and neck held forwards,
- ache or fatigue across the upper or mid‑back after sitting or standing upright for a while,
- stiffness when you try to straighten up, with a feeling of being “pulled forwards”,
- difficulty finding a comfortable position for reading, screen use or household tasks without slumping.
In more marked cases, there may also be height loss, a sense of imbalance, or difficulty lifting the head to look ahead when walking.
What is happening in the spine
In kyphosis, the thoracic spine curves forwards more than usual. This can happen gradually due to:
- age‑related changes and loss of muscle strength,
- weakness in the back extensor muscles that normally help hold you upright,
- osteoporotic compression fractures, where the front of some vertebrae partly collapse and become wedge‑shaped (shorter at the front than at the back),
- changes in discs, joints and ligaments that allow or encourage more forward bend.
The increased curve means:
- more load is taken on the front of the vertebrae and discs,
- the back extensor muscles have to work harder, especially near the base of the neck and between the shoulder blades,
- ligaments and joint capsules at the back are held under tension.
Over time, this can make the area ache and tire more quickly and can reduce how easily you can straighten from a rounded posture. If several vertebrae have become wedge‑shaped after fractures, the curve may be more fixed and less reversible.
Who tends to develop kyphosis
An increased kyphotic curve is more likely in:
- older adults, particularly post‑menopausal women,
- people with osteoporosis and vertebral compression fractures,
- adults who have spent many years in flexed postures (for example, sustained forward‑bent work or habitual slumping),
- those with specific conditions affecting spinal shape in childhood or adolescence.
Many people with an increased thoracic curve do not have significant pain. When pain is present, it usually reflects a mix of joint, disc, muscle and ligament strain around the curved area and, in some cases, around the neck and lower back as they try to compensate.
Why kyphosis can affect function
Beyond pain, kyphosis can:
- make it harder to look straight ahead when walking if the head and neck are flexed forwards,
- affect balance by moving your centre of mass forwards,
- reduce the amount of space in the chest for the lungs to expand if the curve is very pronounced,
- change the way the lower back and neck are loaded as they compensate for the increased mid‑back curve, sometimes leading to secondary pain in those regions.
Milder curves can often be managed with postural training, strengthening and sensible set‑up changes. More severe or rapidly changing curves, especially with height loss or suspected fracture, need medical assessment.
Practical changes that often help this kind of back pain
If kyphosis is part of your pain, it often helps to:
- use back support and occasional cushions so you sit with your upper back supported rather than hanging in a deep slump,
- bring reading material, screens and work closer to eye level so you do not have to bend your head and upper back as far forwards,
- work on strengthening the upper‑back and shoulder‑blade muscles that help you gently straighten and hold a comfortable upright posture,
- keep the hips and lower back mobile and strong, so they do not have to over‑compensate for the thoracic curve.
These steps reduce the time your mid‑back spends under high strain and build the muscular support that helps hold you nearer to a more comfortable posture. The general principles described earlier on the main page — staying active, breaking up long static positions and working on strength — also support this.
How this brace can help if you have kyphosis‑related pain
In kyphosis‑related pain, the mechanical problems are an increased forward curve of the thoracic spine, extra load on the front of the vertebrae and discs, and fatigue and strain in the upper‑back muscles that are trying to hold you up. A brace can help if it:
- provides gentle encouragement towards a more upright thoracic posture,
- reduces deep, prolonged slumping,
- spreads contact across the upper and mid‑back instead of concentrating load in one area.
The BackReviver Posture Support Back Brace does this through its full‑length back panel, which reaches from the lower back up into the mid‑back between the shoulder blades, and its flexible shoulder and side straps. As you begin to slump, the panel and straps tighten slightly and gently resist that movement, prompting you to bring your chest and head back. By supporting a slightly less curved posture within what is comfortable and safe for you, the brace shifts some load back from the very front of the vertebrae and discs towards a more shared distribution, and reduces how hard the upper‑back extensor muscles have to work just to hold you upright.
Using the brace if kyphosis is part of your pain
If an increased upper‑back curve is part of your pain:
- use the brace when you are likely to be sitting or standing for long periods, such as desk work, long conversations, or standing in queues,
- adjust the shoulder and side straps so you feel a gentle reminder to stay more upright, not a forced, rigid position,
- combine brace use with strengthening work for the upper‑back and shoulder‑blade muscles and with sensible set‑up changes (such as raising reading material and screens).
The brace should feel like a support and reminder, not a device forcing you bolt upright. If you notice new, severe pain, rapid height loss or symptoms that suggest a new fracture or serious disease, seek assessment promptly rather than trying to manage things yourself with the brace.
For Thoracic Postural Pain (Upper‑Back Desk‑Related Ache)
What thoracic postural pain usually feels like
Thoracic postural pain refers to ache and fatigue in the upper or mid‑back, often linked to prolonged sitting or standing in a rounded posture. People commonly describe:
- a dull ache or burning feeling between the shoulder blades or across the mid‑back,
- tightness across the shoulders and upper back after long desk work, reading or looking down,
- a sense of “knots” or stiffness that improves for a while when they move or stretch,
- discomfort when trying to sit or stand upright after being slumped.
You may recognise the feeling of your upper back starting to burn or feel knotted — a tight, tired ache between the shoulder blades — after a long spell at a desk, then easing for a while when you stand up and move. This can be frustrating, especially when your work or daily responsibilities involve long periods at a desk that are difficult to change. The aim is to help your back cope better with those demands, rather than to avoid sitting altogether.
What is happening in the upper back
In prolonged slumped sitting or standing with the head and shoulders forwards:
- the thoracic spine flexes (curves forwards) more than usual,
- the head often sits forwards of the shoulders,
- muscles between the shoulder blades and along the spine work harder to support the head and upper body,
- ligaments and joint capsules at the back of the spine are held under tension.
Your upper‑back muscles end up doing far more “holding work” than they were designed for, just to keep your head from dropping forwards. Over time, this can lead to tired, overworked upper‑back muscles, stiffness in the joints between vertebrae and where ribs join the spine, and a habitual rounded posture that is easier for the body to slip back into. The combination of muscle fatigue, joint stiffness and stretched ligaments is why the area can feel sore, tight and difficult to straighten.
Who tends to develop thoracic postural pain
This kind of upper‑back pain is common in people who:
- spend many hours at desks, in meetings or driving,
- use laptops, tablets or phones for long periods with the head and shoulders forwards,
- have weaker upper‑back and shoulder‑blade muscles,
- have workstations or chairs that are not well adjusted.
Many of these factors are part of modern working life, which is why this type of pain is so frequent.
How it affects daily life and why it can persist
Thoracic postural pain can:
- make it hard to sit comfortably through the working day,
- distract you from tasks and reduce concentration,
- limit tolerance for activities such as reading or using a computer,
- lead to a cycle where you feel unable to sit upright for long, so you slump again, which then irritates the area further.
Pain tends to persist when you keep returning to the same prolonged, slumped postures, supporting muscles remain relatively weak, and work and home set‑ups make it difficult to sit or stand upright comfortably.
Practical changes that often help this kind of upper‑back pain
If thoracic posture is part of your pain, it often helps to:
- adjust your desk, screen and chair so that you can sit with your feet flat, hips and knees around right angles, and your eyes roughly level with the upper part of the screen,
- bring work closer so you do not have to bend your head and upper back as far forwards,
- use the back of the chair and, if needed, a small cushion to support a gentle upright posture rather than perching at the front and slumping,
- take regular short breaks to stand up, gently stretch the chest and move the shoulders,
- strengthen the muscles between the shoulder blades and around the upper back with simple, targeted exercises.
Even a small change, like raising your screen so you look slightly forwards rather than down, can noticeably reduce upper‑back strain over a day. Many people also find it helpful to build in regular, brief breaks — for example, standing up or moving for a moment each time they finish an email or a page of reading. These steps reduce the time your upper and mid‑back spend in deep flexion and build endurance in the muscles that hold you more comfortably upright. The general advice described earlier on the main page also supports this.
How this brace can help if you have thoracic postural pain
In thoracic postural pain, the main mechanical issues are an increased forward curve in the upper and mid‑back during slumped sitting or standing, fatigue and strain in the muscles that try to correct or support that curve, and tissues around the thoracic joints being held at or near the end of their flexion range for long periods. A brace can help if it:
- gently discourages deep slumping,
- reminds you when you begin to round forwards,
- spreads contact over the upper and mid‑back instead of digging into one point.
The BackReviver Posture Support Back Brace does this through its full‑length back panel, which runs up into the mid‑back between the shoulder blades, and its flexible shoulder and side straps. As you start to slump, the panel and straps tighten subtly and provide a cue to straighten, sharing some of the work of maintaining a more upright posture and reducing continuous strain on tired muscles and ligaments. This can help your upper‑back muscles fatigue more slowly during long periods at a desk. You may find you can sit upright for longer before you feel the familiar burn or tightness between your shoulder blades.
Using the brace if you have upper‑back postural pain
If upper‑back posture is a clear part of your pain:
- use the brace for the times of day when you tend to slump most — for example, long periods at a desk, extended meetings, or evening screen time,
- adjust the shoulder and side straps so you feel a gentle reminder, not a rigid pull,
- combine brace use with set‑up changes and strengthening exercises so that, over time, you rely more on your own muscle control and less on the brace.
If you notice new, severe pain, breathlessness, chest pain, or symptoms that do not change with posture, seek assessment to rule out other causes rather than trying to manage things yourself with the brace.
For Hyperlordosis (Excess Lower‑Back Arch)
What hyperlordosis usually feels like
Hyperlordosis describes an exaggerated inward curve in the lower back. Some natural curve is normal; hyperlordosis is when that curve is clearly increased. People with this pattern often report:
- a “sway‑back” appearance, with the pelvis tilted forwards and the lower back heavily arched,
- ache or sharp pain in the lower back after standing still, walking or doing overhead tasks,
- tightness in the front of the hips and sometimes the hamstrings,
- fatigue and discomfort in the lower‑back muscles by the end of the day.
Pain may be worse when standing still with weight pushed forwards onto the toes, wearing high heels, or repeatedly doing overhead work without support.
What is happening in the spine and pelvis
In hyperlordosis:
- the pelvis is often tipped forwards (anterior pelvic tilt),
- the lower lumbar vertebrae are extended more than usual, especially at the lumbosacral junction (around L5/S1),
- the facet joints at the back of the spine are more closely compressed,
- the back muscles are working harder to hold this position.
This means:
- the facet joints and joint capsules may be under more pressure in standing and during extension,
- the back‑outer part of the discs and the ligaments at the back of the spine may be strained, particularly at the junction between the lower back and the sacrum,
- muscles at the front of the hips (hip flexors) can shorten and resist attempts to bring the pelvis back towards a more neutral position.
Over time, it can start to feel “normal” to over‑arch, but that “normal” posture keeps parts of the lower back under high strain.
Who tends to develop hyperlordosis
Hyperlordosis is more likely in:
- people who stand for long periods in one place and habitually rest with the hips pushed forwards,
- those with weaker abdominal and buttock muscles and tighter hip flexors,
- some dancers, gymnasts and sports participants who repeatedly extend the lower back,
- people with a larger abdominal mass that pulls the pelvis forwards.
Not everyone with hyperlordosis has pain, but when discomfort is present it is often clearly linked to prolonged standing or extension‑biased tasks.
Why it can persist
This situation can be slow to change because:
- the body becomes used to the over‑arched position as “normal”,
- muscles and ligaments at the front of the hips and the back of the spine adapt to that posture,
- everyday standing and walking continue to load the facet joints and posterior soft tissues in the same way.
If you do not address both posture and muscle balance, the lower back continues to be held nearer the end of its extension range in many activities, keeping tissues irritated.
Practical changes that often help this kind of back pain
If hyperlordosis is part of your problem, it often helps to:
- become more aware of your standing posture and practise bringing the pelvis to a more neutral position — not tucked under, not pushed forwards — so the lower‑back curve is moderate, not exaggerated,
- avoid standing for long periods with weight shifted forwards and hips pushed ahead of the ankles,
- adjust footwear and work set‑up where possible to reduce the need to lean back to see or reach things,
- strengthen your abdominal and buttock muscles and stretch tight muscles at the front of your hips under guidance.
These steps shift the spine away from its extremes of extension and reduce continuous facet and soft‑tissue compression. The more general strengthening and set‑up advice described earlier on the main page also supports this.
How this brace can help if you have hyperlordosis
In hyperlordosis‑related pain, the mechanical problems are excessive extension at the lower lumbar levels and increased compression of the facet joints and the ligaments and capsules at the back of the spine in standing and extension‑biased tasks. A brace can help if it:
- limits how deeply you can arch your lower back, especially in standing,
- encourages a more moderate, neutral lumbar curve during day‑to‑day activities,
- makes you more aware when you start to push your hips forwards and lean back.
The BackReviver Posture Support Back Brace does this by using its semi‑rigid lumbar stays and belt to resist deep extension and its full‑length panel to give feedback when your upper body leans back. Together, these features help reduce the amount of time you spend at the very end of your extension range, where facet joints and supporting ligaments are more likely to be jammed and painful. That can make long, fairly static standing — for example working at a counter or talking in queues — feel less like it is jamming your lower back.
Using the brace if you have an exaggerated lower‑back arch
If an exaggerated lower‑back arch is part of your pain:
- use the brace for activities that tend to bring on symptoms — for example, longer standing spells, jobs with a lot of overhead reaching, or situations where you know you tend to push your hips forwards,
- adjust the belt so you feel firmly supported through the lower back, and notice gentle resistance when you try to arch deeply,
- combine brace use with exercises and stretches aimed at bringing the pelvis and lower back towards a more neutral position.
The goal is not to flatten your lumbar curve completely, but to help you spend more of the day in a comfortable, moderate posture instead of in a deep sway‑back position. If pain worsens, spreads, or is accompanied by leg symptoms such as numbness, weakness or changes in bladder or bowel control, arrange assessment rather than only changing how you wear the brace.
For Scoliosis (Adult)
What adult scoliosis usually feels like
Scoliosis is a sideways curve of the spine, usually with some rotation. In adults, it can be a continuation of a curve that began earlier in life, or it can develop or become more noticeable later on. Not everyone with scoliosis has pain. When it does cause problems, people often report:
- visible asymmetry — one shoulder higher than the other, one hip more prominent, or one side of the ribcage more curved,
- a feeling of one‑sided tightness or ache in the back or one side of the lower back or waist,
- faster fatigue on one side when standing or walking,
- difficulty finding a comfortable position for sitting or standing without leaning to one side.
Pain may be worse after longer periods of standing or walking, or after tasks that involve repeated side‑bending or rotation.
What is happening in the curved spine
In scoliosis:
- the vertebrae tilt sideways and rotate,
- the discs between them become wedge‑shaped rather than symmetrical,
- facet joints are loaded differently on each side,
- in thoracic curves, ribs on one side may be more prominent because of the rotation.
This means:
- muscles and ligaments on the concave (inner) side of the curve can become tight and overworked as they try to hold you upright,
- tissues on the convex (outer) side can be under strain from being lengthened and supporting more of the body’s weight,
- load through the spine and ribcage is uneven when you sit, stand and move.
Over time, these asymmetries can lead to one‑sided pain, fatigue and stiffness, especially if general strength and mobility are reduced.
Types of adult scoliosis and who tends to be affected
In adults, scoliosis is often:
- adolescent‑onset idiopathic scoliosis that has persisted from teenage years and may slowly progress,
- degenerative (“de‑novo”) scoliosis, where age‑related disc and joint changes in the lumbar spine gradually lead to sideways drift and rotation.
Adult scoliosis is more likely to be symptomatic when:
- the curve is moderate to large,
- several discs and joints have significant wear and tear,
- trunk and hip muscles are relatively weak and fatigue quickly,
- there are other issues such as leg‑length differences or long‑standing postural habits that encourage leaning to one side.
Monitoring and medical assessment are important if you notice the curve changing shape, you lose height quickly, or pain and imbalance are increasing.
How adult scoliosis affects function
Scoliosis can:
- reduce how long you can stand or walk comfortably before one‑sided ache and fatigue build up,
- make certain positions — for example, standing with weight more on one leg — particularly provocative,
- lead to one‑sided muscle fatigue and pain in the back, lower back or between the shoulder blades,
- affect balance and confidence in movement if the curve or compensations are more pronounced.
Support does not straighten the curve in adults, but it can help the trunk feel more level and stable and reduce some of the extra effort on one side.
Everyday changes that often help scoliosis‑related pain
If scoliosis is part of your back problem, it often helps to:
- aim for more even weight‑bearing in standing and sitting, rather than habitually leaning to one side,
- adjust work and seating so you are not always rotated or bent towards the curved side,
- strengthen the muscles on both sides of your trunk and around your hips so they can share support more evenly,
- keep the spine as mobile as is comfortable, within limits set by your specialist team.
These steps can reduce one‑sided overloading and support better control around the curved levels. The general strengthening and set‑up advice described earlier on the main page also applies here.
How this brace can help if you have adult scoliosis
In adult scoliosis, the mechanical issues are uneven load through the spine and ribcage, one‑sided muscle fatigue and strain, and a trunk that may feel less stable or “off‑centre”. A brace cannot correct the curve in an adult spine, but it can help if it:
- provides a more even hold around the trunk,
- supports a more level, upright posture within your natural limits,
- reduces the effort needed from overworked muscles on one side.
The BackReviver Posture Support Back Brace does this by:
- using a full‑length back panel that runs along the spine from the lower back into the mid‑back, sharing support across multiple levels rather than gripping a single spot,
- combining this with a broad lumbar belt and semi‑rigid stays, which give a firm but adjustable hold around the waist and lower back,
- using shoulder and side straps to help keep the shoulders and upper back better aligned over the pelvis, rather than drifting further into the curve or collapse.
By spreading support along the curved area and helping you feel more centrally supported, the brace can reduce some of the extra holding work for muscles on the more loaded side and make it easier to stand and sit feeling more centred without trying to force the curve straight.
Using the brace if you have adult scoliosis
If you have adult scoliosis:
- use the brace for activities where one‑sided fatigue and ache are most noticeable — such as longer periods on your feet, walking, or tasks that involve standing in one place,
- adjust the straps so the brace feels even from left to right and you feel gently encouraged towards a more upright, balanced position,
- combine brace use with exercises and any specific advice from your spine specialist or physiotherapist,
- loosen or remove the brace during rest periods and when doing your exercises so your muscles can continue to work.
The aim is not to correct the curve, but to make everyday postures and movements feel more supported and easier to manage over a day. If you notice rapid changes in posture, worsening imbalance, new leg weakness or changes in bladder or bowel control, seek medical advice promptly; do not rely on a brace alone in those situations.
For Spinal Fracture (Osteoporotic Vertebral Compression)
What an osteoporotic vertebral fracture usually feels like
Osteoporotic vertebral compression fractures are small fractures in the spine where the front of a vertebra partially collapses. They are most common in older adults with reduced bone strength. Typical features include:
- sudden onset of sharp, localised back pain, often in the mid‑ or lower thoracic spine, sometimes after a minor strain or even a simple movement,
- pain that worsens with standing and walking and eases when lying down,
- tenderness when the affected area is pressed,
- possible height loss or a new forward stoop over time.
The pain can be severe at first and may take weeks or months to settle.
What is happening in the bone and spine
In osteoporosis, bone density and strength are reduced and vertebral bodies are more vulnerable to collapse, especially at the front. In a compression fracture:
- the front part of the vertebral body collapses more than the back,
- the vertebra becomes wedge‑shaped, with the front shorter than the back,
- the spine bends forwards more at that level.
When the front is shorter than the back in this way, the vertebra takes on a wedge shape. That wedge shape changes how forces are transmitted through the spine, can increase strain on the back of the vertebrae and discs above and below, and contributes to an increased forward curve (kyphosis) if several fractures occur. Pain comes from the fracture itself, the surrounding soft tissues reacting, and the altered mechanics as other levels try to compensate.
Who is at higher risk
Compression fractures are more likely in:
- older adults, especially post‑menopausal women,
- people with known osteoporosis or very low bone density,
- those on certain medications or with conditions that affect bone health,
- people who have had previous vertebral fractures.
Sometimes fractures occur after a specific event such as a fall, lifting or a sudden bend; sometimes they occur with minimal or no clear trauma.
Why they matter and when to seek help
Osteoporotic vertebral fractures matter because they can:
- cause significant pain and temporary disability,
- increase the risk of further fractures (a pattern where one fracture increases the risk of more),
- lead to increased thoracic kyphosis, height loss and balance problems.
Any suspected vertebral fracture should be assessed promptly. A brace sold for mechanical back pain is not a substitute for fracture‑specific braces or for medical management. Treatment plans often include pain management, bone‑strengthening medication and, in some cases, specific spinal supports or procedures.
Seek urgent medical assessment if you suspect a new spinal fracture — for example, new sharp, focal back pain after a fall or even a minor strain in someone with known osteoporosis. These situations should not be managed by simply adding a brace.
Where this brace fits in (and where it does not)
The BackReviver Posture Support Back Brace is not a fracture‑immobilising brace and is not designed for the initial management of acute vertebral fractures. It should not be used for a suspected or recent fracture unless the clinician managing your care has specifically advised that this type of support is appropriate at your stage of recovery.
In some cases, once the fracture has been assessed and managed, healing is underway, and a clinician has advised that a non‑fracture brace is safe to use, a posture support brace can help in a few ways. It can:
- give you a little extra support during lighter upright activities,
- make it easier to avoid very deep forward bends,
- encourage a more upright posture so that strain is shared more evenly along the spine rather than focused just above and below the old fracture site.
Any such use must be tailored to you and timed correctly; in some cases, other specific braces or no brace at all will be more appropriate.
Using the brace if you have had an osteoporotic vertebral fracture
If you have had an osteoporotic vertebral fracture and your clinician has approved this type of brace for your situation:
- follow their guidance on when to start using it and for how long at a time,
- use it for lighter, upright activities where some extra support is helpful and where they have said it is safe,
- ensure it is not so tight or positioned in such a way that it causes new pain or pressure over the fracture area,
- continue to follow advice on bone health, exercise and fall prevention.
If you experience new sharp pain, increasing deformity, or neurological symptoms (such as leg weakness or changes in bladder or bowel control), seek urgent assessment rather than adjusting how you use the brace.
How to choose, fit and use this brace
Measuring and choosing a size
To find your size:
- Stand relaxed and wrap a soft tape measure around your waist at roughly belly‑button level, keeping it level all the way round.
- Pull it snug but not tight and note the measurement in centimetres.
- Use the size chart to choose the size whose range best fits your measurement, using the height notes to judge how far up your back the panel is likely to reach.
The waist measurement is the most important guide when you choose a size. If you fall between sizes, the smaller size will normally give a firmer hold; the larger will feel a little gentler. The height notes help you check that the panel will sit over the areas that tend to hurt, rather than cutting into your ribs or sitting too low over the pelvis.
How it should feel when fitted
When fitted properly, the brace should feel snug and supportive but not restrictive. The top of the panel should sit just below the base of your neck, the lower‑back pad should be centred across your lower back, and the belt should sit comfortably around your waist.
After fastening:
- take a deep breath and slide two fingers under the front of the belt; if you cannot do that easily, loosen the straps,
- check that you can still breathe and move comfortably.
If you need to pull it so tight that breathing feels restricted, movement feels very stiff, or you get soreness or marks that do not fade quickly, ease it off. Over‑tightening will not protect your back better and can make you more uncomfortable.
When and how long to wear it
This brace is intended to support you during the parts of the day that usually trigger your symptoms, not as something to wear very tight from morning to night.
A practical way to start is to:
- use the brace for up to an hour at a time around a task or time of day you already know is difficult — for example, a spell of sitting for work, a block of standing, or a run of household jobs,
- then remove it or loosen it fully for at least a similar length of time.
Over the day, this might add up to a few hours of use, split into several shorter blocks. This gives you help where you need it most, while also giving your muscles and joints time to work and move without support.
If you find you are wearing the brace for most of the day and feel you cannot manage ordinary activities without it, that is a sign to review your overall back care with a clinician. The brace is there to support you through the harder parts of your day while you build strength and confidence, not to become something you feel completely dependent on.
Putting it on and taking it off
To put the brace on:
- Loosen all straps fully.
- Slip each arm through the padded shoulder straps.
- Position the back panel so the top sits just below the base of your neck and the lower‑back pad is centred.
- Wrap the belt around your waist and fasten the front closure.
- Tighten the side straps a little at a time, alternating sides, until the hold feels even and supportive.
To take it off:
- While standing or sitting fairly upright, undo the front closure.
- Loosen the side straps fully.
- Slide one shoulder strap off, then the other, keeping your back in a comfortable position.
If you have difficulty with shoulder movement, balance or coordination, you may need another person to help with these steps.
Safety, important information and when to seek help
This brace is intended for adults with mechanical, posture‑related back pain — in other words, pain that is linked to how you sit, stand and move. It is not designed to diagnose or treat serious underlying disease. Some combinations of back pain and other symptoms can be a sign of a more significant problem. It is important to recognise these and seek appropriate help.
Do not use this brace if:
- you are pregnant,
- you have a pacemaker, implantable defibrillator, cochlear implant, insulin pump, neurostimulator or any other implanted electronic or magnetic device,
- you have had recent spinal surgery, a suspected or confirmed spinal fracture, or very severe osteoporosis, unless the clinician looking after you has specifically said it is appropriate,
- you have broken skin, an active infection or a rash under the area where the brace would sit.
Stop using the brace and seek advice from a GP, physiotherapist or another appropriate clinician if:
- your pain worsens or spreads despite using the brace sensibly,
- your back pain changes suddenly and feels very different from your usual pattern,
- you develop new numbness, tingling or weakness in one or both legs,
- you notice persistent redness, sore areas or rubbing despite adjusting fit and tension.
Symptoms that may indicate severe nerve compression
Some symptoms suggest that nerves in the lower spine may be under significant pressure. This can sometimes be due to conditions such as a large disc prolapse or severe narrowing in the spinal canal (cauda equina syndrome). These situations are uncommon, but they need urgent assessment because delayed treatment can increase the risk of permanent nerve damage.
Seek same‑day urgent medical assessment — for example at an emergency department or urgent assessment service — if you notice:
- new difficulty controlling your bladder or bowels, or not realising when you need to go,
- numbness or loss of feeling in the groin or inner buttocks (the “saddle” area),
- rapidly worsening weakness in one or both legs, or difficulty lifting the foot when walking,
- severe back pain after a fall, crash or other significant injury, especially if you also notice leg symptoms.
These symptoms are not things to manage yourself with a brace or exercises. They need urgent medical assessment in hospital or an emergency service so that the cause can be identified and, if necessary, treated promptly.
Symptoms that may indicate fracture, infection or other serious problems in the spine
Back pain is most often mechanical and not due to serious disease. Sometimes, however, it can be linked to a fracture, an infection such as a spinal abscess or bone infection (osteomyelitis), or other less common but more serious conditions affecting the spine. These are much less common than everyday back pain, but they do occur, especially in people with certain risks. Treatment is very different to treatment for simple mechanical pain and usually needs medical supervision.
Arrange a prompt medical check‑up with a GP or urgent care service if you notice:
- back pain that started after even a minor fall or twist, particularly if you know you have osteoporosis or fragile bones,
- new back pain in someone with a history of significant long‑term illness, especially if the pain is constant, severe, or worse at night,
- back pain with feeling generally unwell, fever or chills,
- unexplained weight loss with new back pain,
- back pain that is steadily getting worse over weeks, especially if it does not ease with rest or simple measures.
These groups of warning signs do not always mean there is a serious underlying problem, but they do warrant proper medical review. A doctor may arrange tests such as blood tests or scans, or refer you to a specialist, to rule out or treat conditions that need specific management.
Remember: serious conditions do not always show textbook symptoms
Most back pain is mechanical — in other words, linked to how you move and load the spine — and not caused by serious disease. The warning signs above are there to highlight situations where it is sensible to have a medical review rather than trying to manage things yourself with a brace or exercises.
Serious conditions do not always show every “textbook” symptom, or they may show only a few features at first. If you have back pain that is persistent, clearly getting worse, or you are worried for any reason — especially if you have risk factors such as known osteoporosis, a history of significant long‑term illness, or marked weight loss or general illness — it is usually worth discussing it with a GP, even if you do not have every warning sign listed. A clinician can then decide whether further tests or referrals are needed.
If you are unsure whether your symptoms match any of these descriptions, or you are simply worried about how things are going with your back, it is always reasonable to speak to a GP for advice. You do not have to work this out on your own.
Is this brace likely to help you?
This brace is most likely to help if your back pain:
- builds when you sit or stand in one position for a long time,
- eases, at least for a while, when you move or change position,
- is clearly worse with deep slumps, strong backward arches or awkward twisting,
- and has not responded well to very soft or minimal supports alone.
This brace combines a firm lumbar belt and pad, a full‑length back panel, semi‑rigid stays (firm strips that add support) and adjustable shoulder and side straps. Together, these features are designed to:
- help you keep to a more comfortable, fairly straight posture,
- reduce time spent in the positions and movements that usually make your pain worse,
- share support along your back so one sore area is not always taking the strain,
- help you feel more steady and in control when you sit, stand, reach or do light lifting.
If you use it during the parts of your day that usually trigger your symptoms — for example long spells at a desk, standing for extended periods, or household tasks that normally leave you stiff and sore — and alongside the movement, strengthening and simple posture and set‑up changes described earlier, it can help many people find that ordinary activities cause less build‑up of pain and stiffness. Simple steps such as adjusting your chair and screen height, using your chair’s backrest or a cushion for support, and breaking up long sitting spells work well with the brace. It does this by helping you stay nearer the comfortable middle of your movement, by cutting down the time you spend in the deep slumps and strong arches that usually aggravate posture‑related pain, and by sharing some of the holding work that your muscles have been doing without support.
It is not a cure, but it can be a useful tool while you work on the underlying mechanical causes of your pain with appropriate advice and, if needed, with help from a GP, physiotherapist or another clinician.
The information on this page is general guidance, not a personal diagnosis or prescription for you as an individual. Everyone’s back is different, so no specific outcome can be guaranteed, and people’s responses vary. If you are unsure how this brace fits with your diagnosis or with the stage of recovery you are in now, it is sensible to discuss it with a clinician who knows your situation. If the description above matches the type of back pain you experience, and you are looking for more structured support than very soft belts or simple cushions can provide, this brace may be a helpful next step as part of your overall plan.






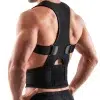
by Mo khan
You cannot go wrong with this back brace. Fits perfectly, very comfortable to wear and supports my back really well. 🙂
by Jack
Took a little bit longer than expected to arrive but was definitely worth the wait.
by Frank Shotter
Good support.
by Phil
I recently purchased this posture corrector because I’ve been having some back trouble. And let me tell ya, it’s been worth every cent!
It’s obviously a quality product. The construction is sturdy and it’s held up beautifully despite daily use. The fit is just right and it’s so comfortable, I sometimes forget I’m wearing it.
But the best part is, it actually works! My back pain has decreased and my posture has improved.
The cost is totally justified by the comfort and benefits it provides. It’s also really easy to use, which is a bonus.
I’m just super happy with this purchase and would definitely recommend this product. It’s made a noticeable difference in my posture and back health.