No products in the cart.
Gel Cushion Ball of Foot pads for Metatarsalgia, Sesamoiditis, Morton’s Neuroma, Arthritis, Calluses & Blisters
£10.49inc VAT
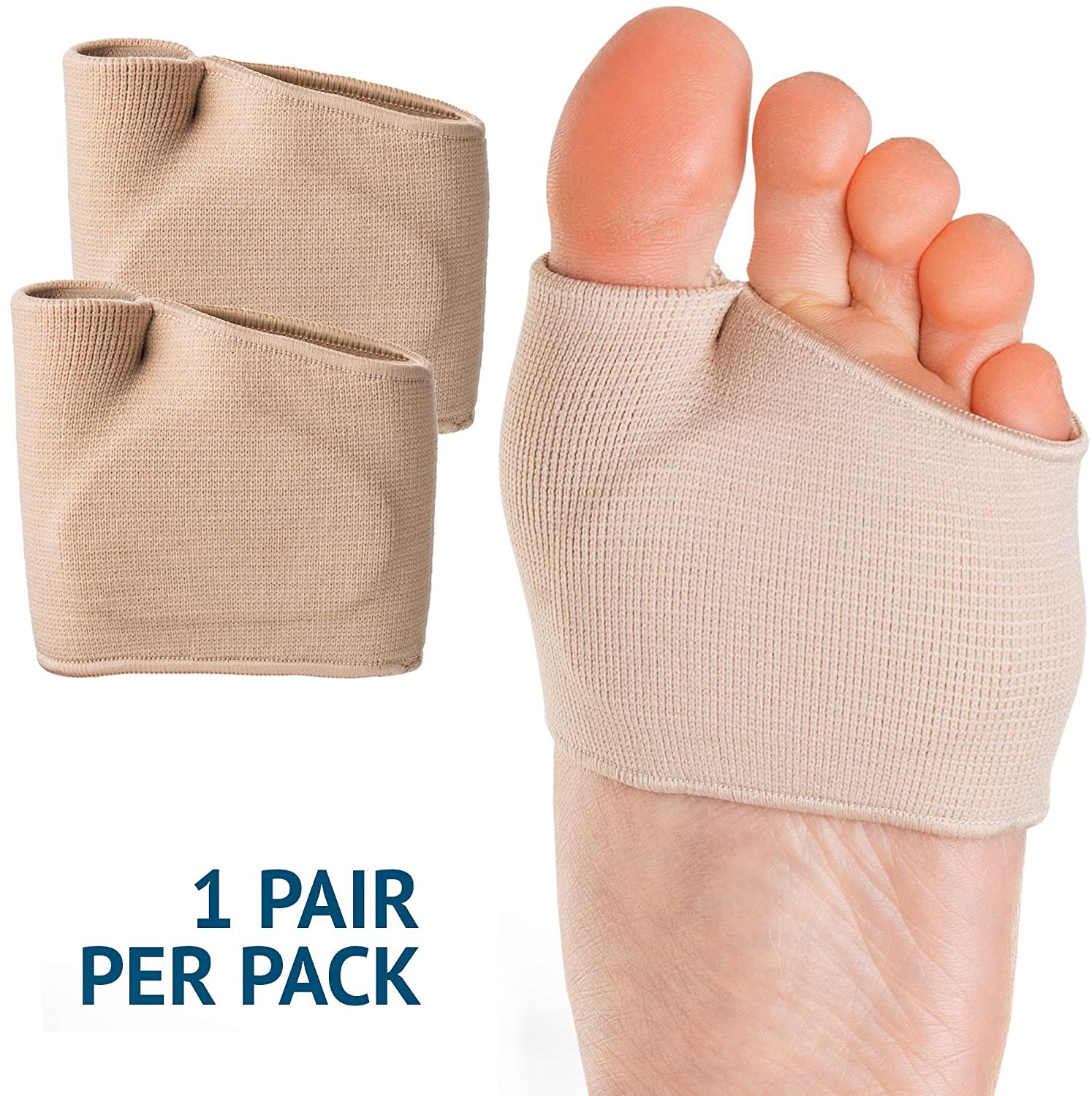
- 2 × FootReviver Gel Cushion Ball of Foot Pads – soft forefoot sleeves with a built‑in gel pad that sits under and just behind the ball of your foot.
- Two adult size ranges: Small (approx. UK 3–7) and Large (approx. UK 7–11). Each sleeve can be worn on either the left or right foot.
- Unisex design intended for adults with pain or soreness under the ball of the foot that flares when standing or walking on hard floors or in thin‑soled shoes.
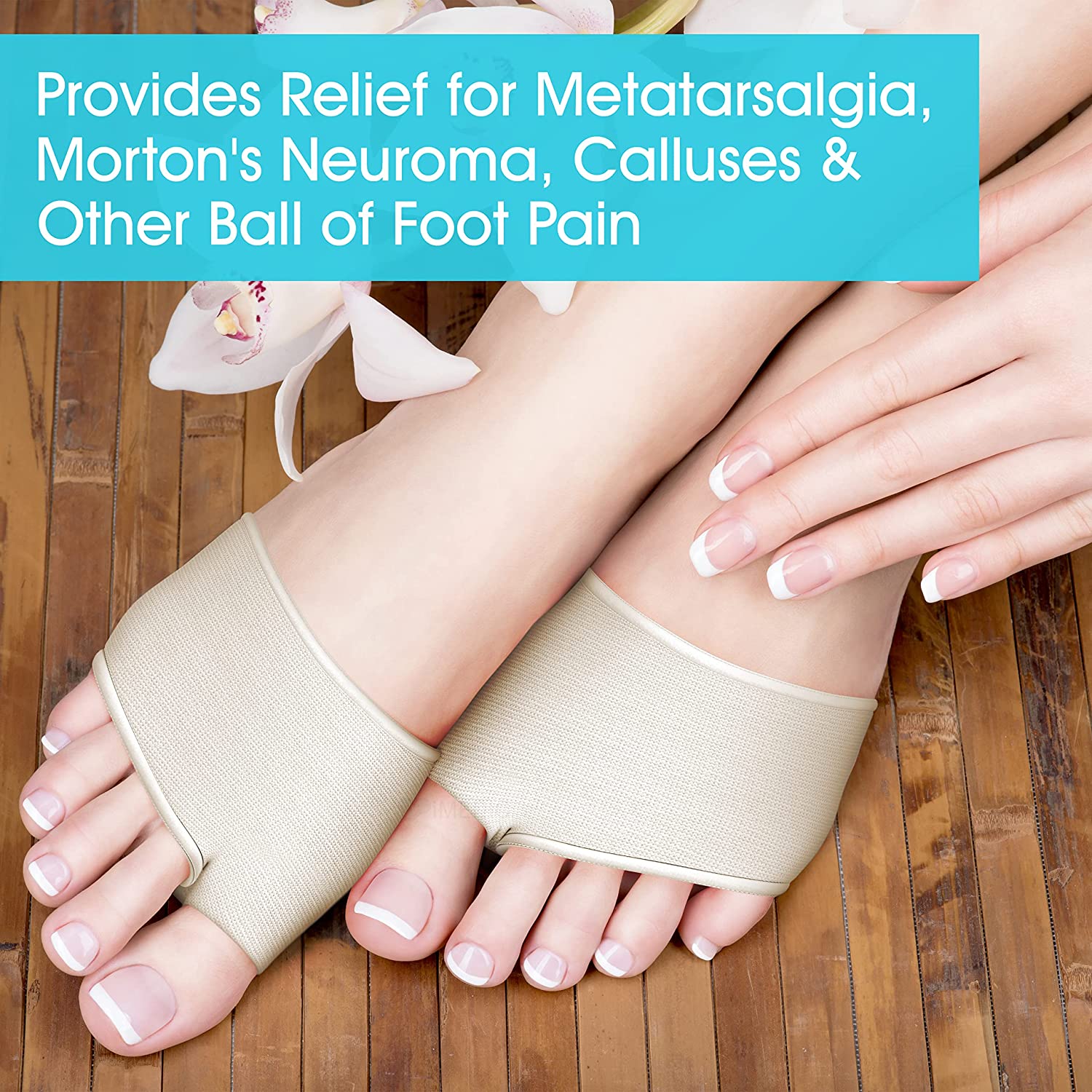
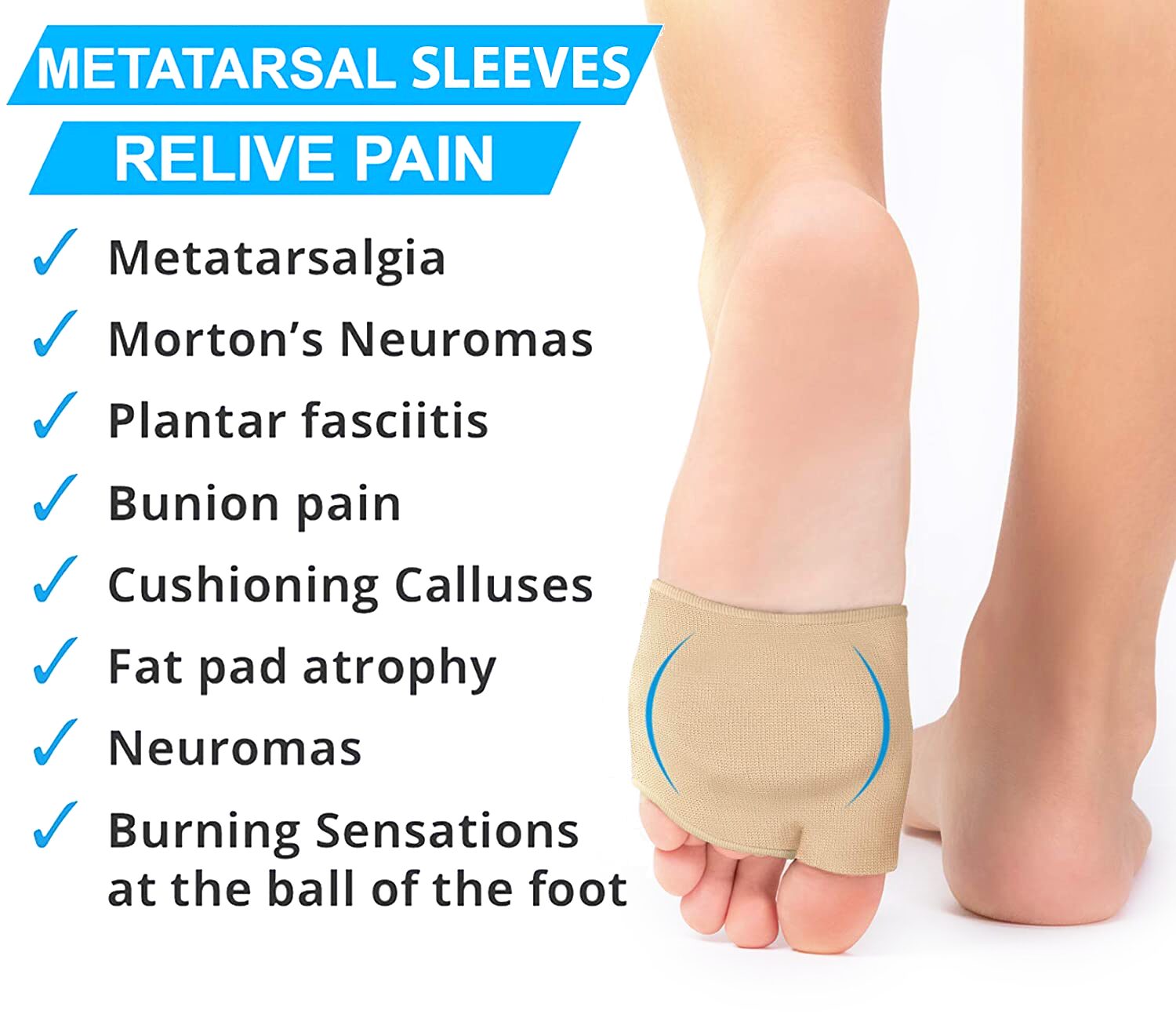
- Suitable for metatarsalgia, Morton’s neuroma‑type symptoms, bunion‑related overload, thinning of the natural fat pad, capsulitis at the lesser toe joints and mild sesamoiditis under the big‑toe joint.
- Contoured gel cushions and supports the area under and just behind the metatarsal heads, helping to reduce sharp pressure on sore spots and support the small arch across the ball of the foot.
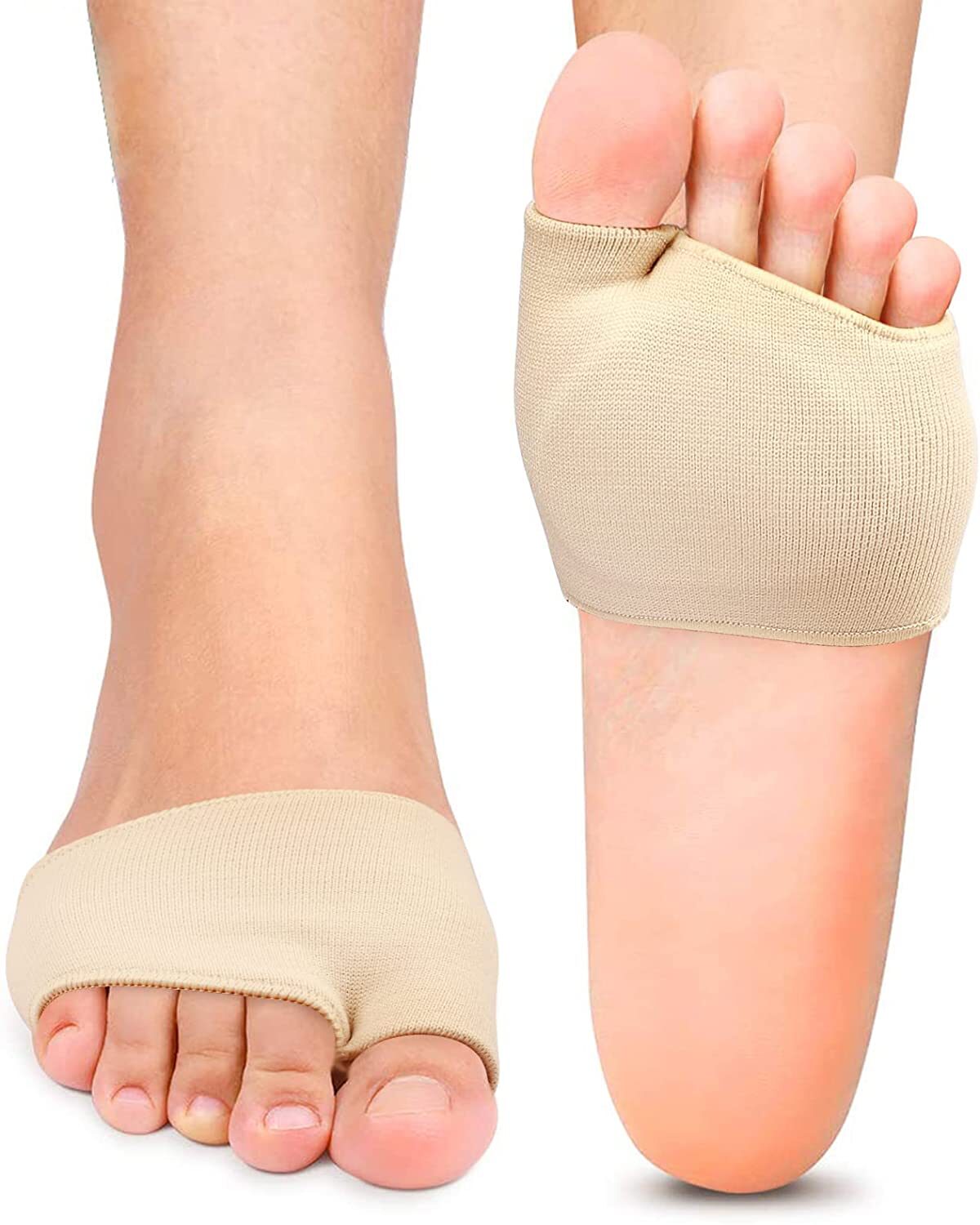
- The smaller sleeve for the big toe and the larger sleeve for the rest of your toes keep the pad correctly positioned as you move, instead of letting it slide forwards or backwards inside the shoe.
- Soft fabric over the gel feels comfortable against the skin, helps reduce rubbing and hotspots, and makes it easier to wear the pads for longer periods.
- Slim profile designed to fit inside most everyday shoes that have a little room in the forefoot, so you can use them at work, when out and about, or at home in the shoes you already wear.
- Worn directly against the skin, with socks over the top if you wish; hand‑washable to help them keep their shape and cushioning.
- Backed by a 30‑day money‑back guarantee so you can judge how they feel in your own shoes and usual activities.
FootReviver Gel Cushion Ball of Foot Pads are soft, sleeve‑style supports for adults with ongoing, load‑related pain or tenderness under the front of the foot. Each sleeve sits around the forefoot with a built‑in gel pad positioned under and just behind the ball of the foot. The smaller sleeve for the big toe and the larger sleeve for the rest of your toes help keep the pad correctly aligned as you move. The aim is to make standing and walking on hard surfaces more comfortable by redistributing pressure away from sore spots under the metatarsal heads and adding extra cushioning where your foot naturally takes the most load.
When every step feels like you’re treading on a stone
Have you ever felt as if you’re constantly stepping on a marble or a small stone, even when there’s nothing in your shoe? Do you get a burning or sharp pain in the ball of your foot that flares when you stand, walk, or go barefoot on a hard floor?
It isn’t just the pain itself that causes problems – it is the way it limits what you can do. You may find yourself cutting walks short, avoiding certain shoes, or thinking twice before heading out because you know your forefoot will pay for it later. Standing at work, getting around the shops, or even moving about at home can start to feel harder than it ought to be.
When this kind of load‑related pain under the ball of the foot has been there for a while, it is often called metatarsalgia. Understanding what is happening under the front of your foot when this occurs helps explain why the pain behaves the way it does and why changing what is directly under that sore area – with a sleeve‑style metatarsal pad such as our FootReviver Gel Cushion Ball of Foot Pads – can make standing and walking more tolerable.
What is happening in the forefoot with metatarsalgia?
Metatarsalgia is a descriptive term rather than a single disease. It refers to pain and tenderness under the front of the foot that is related to repeated loading of the area where the long bones of the forefoot – the metatarsals – meet the toes. This is the region commonly called the ball of the foot.
In that small area you have several important structures packed closely together:
- The rounded ends of the metatarsal bones (metatarsal heads), which act as small “knuckles” under the toes.
- A specialised fatty cushion (the plantar fat pad) beneath them, which spreads impact and protects deeper tissues.
- The joints where the metatarsals meet the toes (metatarsophalangeal or MTP joints), surrounded by a capsule and ligaments.
- Small nerves (interdigital nerves) that run between the metatarsals towards the toes.
- Soft tissues on the sole of the foot, including the front part of the plantar fascia – the band of tissue tying the heel to the toes.
When you walk, your body weight moves from the heel, through the midfoot, and onto the ball of the foot before the toes finally leave the ground. The plantar fat pad under the metatarsal heads deforms and rebounds, absorbing some of the impact and spreading the rest across a relatively wide area. The metatarsal heads and the small arch across the ball of the foot work together so that no single point has to cope with all the force.
In this context, “load” means the combination of your body weight, the impact of each step, and how long you spend on your feet. Metatarsalgia often appears when this system is asked to cope with more load than it can comfortably share out, or when one or more parts of it are not working as they should. Common situations include:
- The fat pad under the ball of the foot becoming thinner or slightly displaced with age, repeated impact, or previous overload, so there is less natural cushioning between bone and ground.
- One or more metatarsal heads sitting lower or taking more weight – for example, because of foot shape, a long second toe, bunions at the big‑toe joint, or changes in toe position.
- Spending long periods on hard surfaces in shoes with thin or worn‑out soles, so there is very little extra cushioning under the forefoot.
- Irritation of the small nerves between the metatarsals, particularly in conditions such as Morton’s neuroma, where a nerve thickens and becomes more sensitive to compression.
In all of these examples, the same thing is happening at tissue level: the same small area under one or more metatarsal heads is exposed to higher pressure than it can comfortably tolerate, step after step. The tissues under and around that spot respond with local inflammation – fluid and inflammatory chemicals build up in the fat pad and joint capsule, and the small nerves become more irritable. The fat pad and capsule tend to produce a bruised or aching sensation, while irritated nerves are more likely to produce burning, tingling, or sharp pains. The discomfort often builds as the day goes on or with repeated activity.
Over weeks and months, if the same small area keeps taking more than its fair share of load, it can become increasingly sensitive. Shorter periods on your feet then start to trigger the same level of pain that previously only appeared after a long day. At this stage, many people start to look for ways to change what is happening under the ball of the foot – through footwear, activity changes, or targeted supports such as a metatarsal pad sleeve.
How the forefoot works during walking
Each step you take can be broken into three broad phases:
- The heel usually meets the ground first (heel strike).
- Weight moves forwards as the foot flattens towards the middle (mid‑stance).
- Finally, the heel lifts and you push off through the ball of the foot and toes (push‑off).
The ball of your foot works hardest during that final push‑off phase. Your body weight is mostly over the front of the foot, and the toes are bending upwards at the MTP joints. The metatarsal heads press down into the shoe or floor, and the fat pad under them is compressed.
On a softer surface, in supportive footwear with decent cushioning, and with healthy tissues, this load is spread and absorbed. On a hard surface, in thin‑soled shoes, or when the natural fat pad is reduced, the same forces are concentrated into smaller, more sensitive areas.
If one or two metatarsal heads are lower or more prominent than the others, they tend to take the brunt of the load at push‑off. A relatively long second metatarsal means the second metatarsal head meets the ground earlier and more firmly. A bunion at the big‑toe joint can reduce the big toe’s ability to share load, shifting more force towards the second and third metatarsals. Changes in arch shape can alter how the front of the foot meets the ground, causing the inner or outer metatarsals to bear more weight.
Each step then repeats the same pattern of extra pressure under those overloaded points. Pain is often sharpest when you first push off after standing still, when walking quickly, or when going upstairs, all of which emphasise the push‑off phase. To avoid this, many people shorten their step, avoid bending the toes fully, or roll towards one edge of the foot. While this can reduce immediate pain at one spot, it can also spread strain to other joints and soft tissues over time.
Common symptoms and who is more at risk
People with metatarsalgia‑type pain usually describe a recognisable group of symptoms. Pain is typically felt under one or more of the metatarsal heads, often in a line just behind the toes. It is usually worse on hard or uneven surfaces than on softer ground, and more noticeable in thinner, less cushioned shoes than in shoes with more supportive soles. Symptoms often build during or after longer periods of standing, walking, or running, and ease when you sit down or take weight off your feet.
The discomfort may start as a dull ache that builds with activity. In more established cases, it can become a sharp, stabbing, or burning pain that appears more quickly and takes longer to ease once aggravated. Some people notice tingling or numbness in one or two toes, especially if a nerve between the metatarsals is irritated. Others see callus forming under the ball of the foot, where the skin has responded to repeated extra pressure.
Certain things make this kind of pain more likely over time. Flat feet can allow the front of the foot to spread and collapse, overloading central metatarsals, while very high arches often mean less cushioning through the midfoot and more direct load on the heel and ball of the foot. Bunions at the big‑toe joint, clawed or hammered toes, and stiffness at the big toe can all shift or concentrate pressure onto particular metatarsal heads. Regularly wearing shoes with minimal cushioning, thin or rigid soles, or narrow fronts that crowd the toes can increase stress under the ball of the foot. High‑heeled shoes move a large share of body weight forwards, so the forefoot carries more load. Jobs or hobbies that involve long hours of standing or walking, particularly on hard floors, expose the forefoot to repeated impact. As you get older, the natural fat pad under the ball of the foot can also become thinner and less resilient.
Of course, not everyone with these foot shapes or habits develops pain, and some people develop problems without obvious risk factors. But these features help explain why certain feet and daily demands are more vulnerable. They also explain why management usually focuses on both reducing the overall load on sore structures – for example, by adjusting shoes or time on hard surfaces – and improving how that load is shared across the front of the foot. Metatarsal pad sleeves such as our FootReviver Gel Cushion Ball of Foot Pads are one way of improving how pressure is shared under and just behind the ball of the foot.
Why a metatarsal pad sleeve can make walking more manageable
A metatarsal pad placed just behind and under the ball of the foot changes how pressure is shared between the metatarsal heads and the surrounding soft tissues at the moment when load is highest. Instead of one or two points taking most of the force at push‑off, more of the front of the foot is brought into contact. This reduces the highest pressure on individual sore areas and adds an extra layer of cushioning on top of the natural fat pad.
A sleeve‑style design goes further than a loose pad. Rather than relying on friction inside the shoe to keep the support in place, a forefoot sleeve wraps around the front of the foot itself. The smaller sleeve for the big toe and the larger sleeve for the rest of your toes help anchor the gel pad in a stable position so that, as your foot rolls from heel to toe, the cushioning moves with you. The elastic fabric adds a modest degree of compression across the ball of the foot, gently hugging the tissues around the metatarsal heads. This can help limit excessive spreading of the forefoot and may feel more supportive when there is mild swelling or fatigue by the end of the day.
Because the pad is held directly against the skin, it can act consistently whether you are wearing shoes or, in some situations, walking barefoot on smoother indoor floors for short periods. Most people use pads like our FootReviver sleeves alongside other measures such as footwear changes, adjusting how long they spend on hard surfaces, and, where appropriate, insoles or orthotic devices that address overall foot posture. They do not replace a proper assessment if your symptoms are severe or hard to explain, but they do give you a direct way to change what is happening under that sore area.
How our FootReviver Gel Cushion Ball of Foot Pads work on your feet
Gel cushioning under and behind the ball of your foot
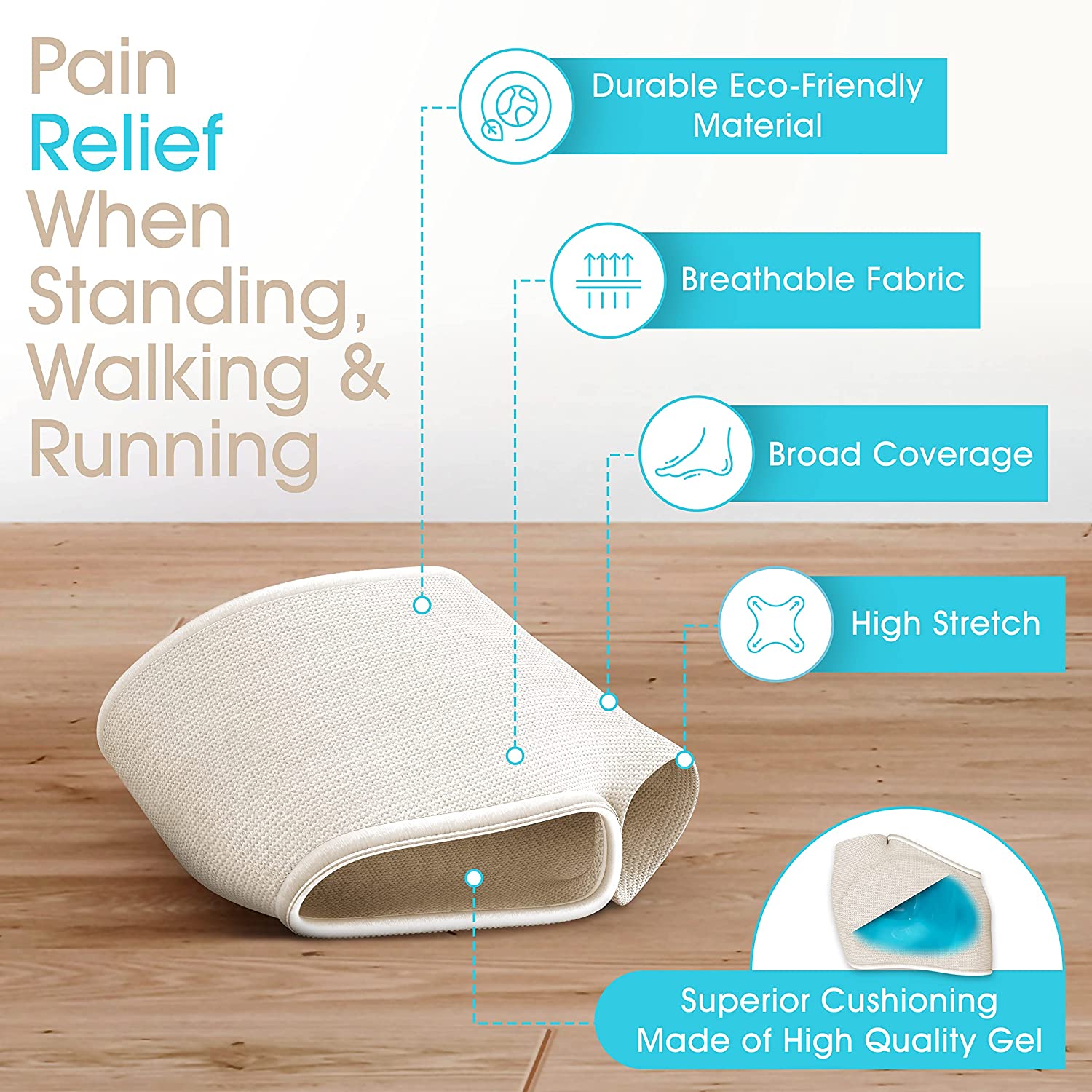
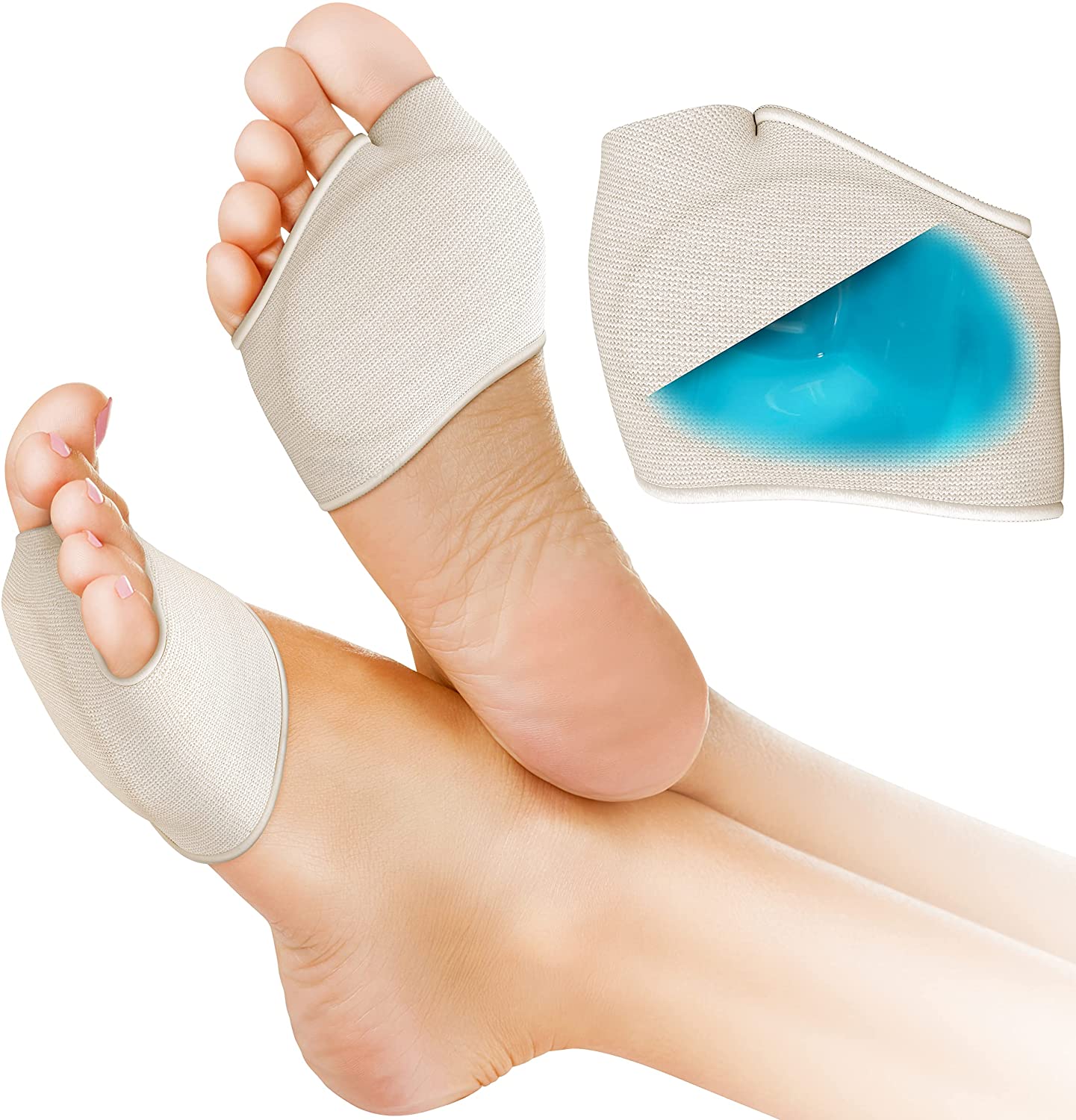
At the heart of our design is a built‑in gel pad, around 3–5 mm thick at its highest point, set into the fabric of the sleeve. It is shaped to sit slightly behind and under the metatarsal heads rather than directly under the toes or back in the arch – exactly where pressure peaks during the push‑off phase of walking.
The gel is firm enough to hold its general contour under load, yet deforms slightly to absorb part of the impact when your forefoot meets the ground. A very soft gel would simply flatten and offer little support; a very hard insert would not cushion well. When you stand or walk, instead of one or two metatarsal heads pressing sharply into a hard surface, the gel spreads that force over a broader area. This reduces peak pressure on individual sore points and adds an extra layer of cushioning over the plantar fat pad.
Because the gel sits inside a sleeve rather than as a loose insert, it stays in line with the ball of your foot rather than sliding forwards under the toes or backwards into the midfoot. Having the pad in the same place on every step is important, because the pressure is always hitting the same spots.
Supporting the small arch across the front of your foot
Across the ball of the foot runs a smaller arch, often called the transverse arch. It spans from the first to the fifth metatarsal and helps keep the front of the foot in a compact, slightly domed shape. When this small arch is supported, the metatarsal heads tend to share load more evenly. When it flattens and the front of the foot spreads outwards and downwards (forefoot splay), one or two metatarsals can drop and act as isolated pressure points.
The contour of the FootReviver gel pad is designed to sit under this transverse arch area. As your foot loads, the pad gently supports this small arch rather than allowing it to collapse fully. At the same time, the surrounding sleeve encourages the front of the foot to stay slightly gathered instead of spreading excessively. This can reduce the tendency for one or two metatarsal heads to take most of the force, especially in flatter or more flexible feet and in the presence of bunions where the big toe’s reduced role shifts weight onto the lesser toes.
By backing up the transverse arch, the pad helps smooth out how weight is shared between the metatarsal heads. If you have developed central forefoot pain or callus under specific metatarsals, this support can ease the feeling that all the weight is going through one bone at the front of your foot.
Forefoot sleeve and toe sleeves for stable positioning and light compression
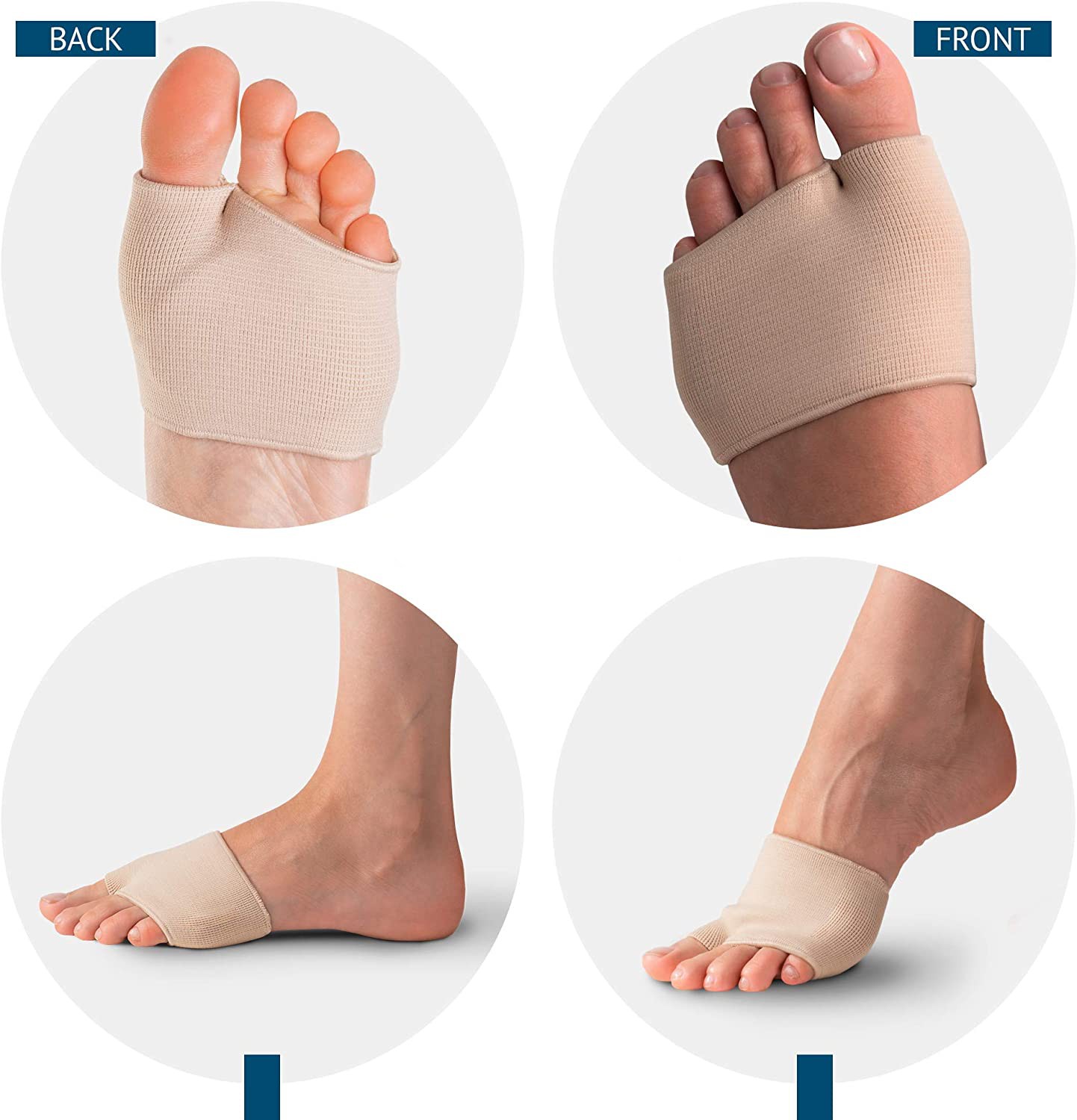
The gel pad is held in place by a soft, stretchy sleeve that slips over the front of your foot. There is a smaller sleeve for the big toe and a larger sleeve that sits around the other toes together.
The smaller sleeve comes part way up the big toe and provides gentle compression, creating a small amount of separation between the big toe and the other toes. The larger sleeve comes part way up the remaining toes as a group, lightly hugging them rather than gripping each toe individually.
This design keeps the pad in line with the ball of your foot, rather than relying on friction against the inside of the shoe. As your foot moves through each step, the sleeve moves with the skin, so the gel remains under and just behind the ball of the foot instead of creeping forwards under the toes or backwards into the arch. That steady positioning matters most when you walk more quickly, go up and down stairs, or change direction, because the ball of your foot is then being loaded from different angles.
The elastic fabric also provides a modest degree of compression around the metatarsal region. It gently hugs the soft tissues – skin, fat pad, small muscles, ligaments and joint capsules – that can feel strained in metatarsalgia. This light squeeze can help limit how much the forefoot spreads with each step and, for some people who notice a sense of fullness or mild swelling around the ball of the foot by evening, can contribute to the area feeling better supported and less tired.
Soft fabric over the gel to protect your skin
The gel pad is fully enclosed inside a soft, elastic fabric rather than being in direct contact with the skin. This means the underside of your foot rests against a smooth textile surface rather than bare gel. The knit has enough stretch to move with both the underlying pad and the skin, avoiding hard edges or abrupt changes in thickness that could rub.
Because this fabric sits directly on the skin, it needs to handle moisture and friction sensibly. The knit structure allows some air movement around the forefoot and helps manage sweat inside closed shoes. By reducing the build‑up of moisture and smoothing the contact between foot and footwear, the sleeve lowers the risk of hot spots, blisters, and areas of irritation developing over bony prominences or callused skin.
If your skin is already tender from pressure, or you are prone to callus or blistering under the ball of the foot, this combination of cushioning plus a gentler contact surface can make the area feel less sore and easier to manage. It allows the pad to be worn for longer periods without the pad itself becoming a new source of rubbing.
Flexible sizing and a slim design for everyday footwear
FootReviver Gel Cushion Ball of Foot Pads come in two size ranges, intended to cover typical adult shoe sizes rather than relying on a single universal fit. The sleeve is symmetrical, so each unit can be used on either left or right foot. If you are between sizes and have a wider forefoot, choosing the larger size is usually more comfortable; if your feet are narrower, the smaller size often gives a closer fit.
The gel and fabric are kept slim enough that the extra depth under the ball of the foot is modest. There is only a limited amount of space in the front of most shoes; if a pad is too thick or rigid, it can crowd the toes against the top or front of the shoe and create new pressure points. Our design aims to provide enough cushioning and lift to change pressure patterns without making your shoes feel tight or awkward.
In practice, this means many people can use the pads in the footwear they already own, provided the shoes offer a reasonable amount of room in the forefoot. Very tight or narrow shoes are usually unsuitable, especially in conditions such as Morton’s neuroma or bunions where cramped footwear is a known irritant. It is also straightforward to move the pads between different pairs of shoes across the week, which can be important for maintaining consistent support.
Built to keep their shape, with a discreet look
A forefoot pad must not only feel comfortable on first use; it also needs to maintain its shape and function over time. The gel used in FootReviver pads is chosen for its ability to deform under load and then recover rather than flatten permanently. The surrounding knit fabric and seams are designed to tolerate repeated stretching as the sleeve is put on and taken off and as your foot moves during daily activity.
This helps the pad keep its shape and support so it behaves in the same way each time you wear it. A gel layer that collapses quickly or a sleeve that loses its elasticity can allow the metatarsal heads to drop back into previous pressure patterns. By resisting this, our design aims to keep the support effect more consistent from day to day.
The sleeve follows the outline of the forefoot and toes, keeping additional bulk to a minimum. This relatively discreet appearance means the pads are not obvious under most closed shoes and, for some people, can be used barefoot indoors without feeling conspicuous. In some open‑fronted footwear they may be used if there is enough space and the shoe does not pinch, although this should always be judged by comfort and stability rather than appearance alone.
Stays put when you move
Forefoot pain rarely appears only when you are standing still. It often flares most during movement: taking the first few steps after getting up, walking at a brisker pace, changing direction, or going up and down stairs. In these situations, the ball of the foot not only takes weight but also experiences changing forces as your body moves over it.
The combination of a contoured gel pad, elastic sleeve, and toe sleeves is designed to stay in place even when your forefoot is working harder. As your foot rolls forwards from heel to toe, the gel remains under and just behind the ball of the foot rather than lagging behind or sliding forwards under the toes. When turning or changing direction, the sleeve helps the pad move with the skin, which reduces the likelihood of the pad bunching or forming ridges that could quickly become uncomfortable.
If you have already started to adjust your walking pattern because you are wary of a painful push‑off, this predictability can be reassuring. Knowing that cushioning will be in the same place on each step can make it more comfortable to move back towards a smoother, more natural stride, rather than constantly guarding the forefoot.
Designed to help with all‑day forefoot load
Many people with metatarsalgia or Morton’s neuroma‑type pain find that a short walk is manageable, but symptoms build as the day goes on. The problem is not just the force of an individual step, but the number of times the same area is loaded. Hours on hard floors, standing at work, or running errands can add up to thousands of small impacts on the same sore tissues.
The FootReviver sleeve is intended to help reduce this cumulative stress. The gel pad absorbs part of the impact on each step and redistributes the rest away from the most sensitive points. The compression from the sleeve offers light support to the soft tissues that might otherwise feel progressively more swollen and tired. The fabric lining reduces rubbing, which is particularly important when the skin is under pressure for long periods.
Together, these elements can slow the rate at which forefoot discomfort builds during a typical day by reducing repeated peak pressure on the same areas. This does not mean that pain will disappear completely, particularly in more advanced or complex conditions, but many people find they can stay on their feet for longer before symptoms become intrusive.
Who tends to find these pads particularly helpful?
These pads are designed for adults with ongoing, load‑related pain under the ball of the foot. If your pain sits just behind the toes, flares when you stand or walk on hard floors or in thin‑soled shoes, and tends to ease when you sit down, they may be worth considering.
People who often report benefit include those who have been told they have metatarsalgia, Morton’s neuroma, or “forefoot overload” and want extra cushioning directly under the ball of the foot; those who notice callus or particular tenderness under one or two metatarsal heads, suggesting that these areas are taking more than their share of pressure; those with flatter feet or higher arches who experience forefoot pain after time on hard surfaces; and people whose work or home life involves long hours of standing or walking on firm floors that cannot easily be avoided.
These pads are not intended as a stand‑alone solution for acute injuries such as suspected fractures, severe sprains, or turf‑toe‑type hyperextension injuries, for marked deformities, or for complex systemic conditions such as advanced rheumatoid arthritis or poorly controlled gout. In those situations, medical assessment is essential, and any cushioning or support should be introduced under professional guidance. If you already use prescribed insoles or orthotic devices, it is sensible to discuss any additional forefoot padding with the clinician who supplied them. Used in the right circumstances, FootReviver Gel Cushion Ball of Foot Pads can be one useful part of making everyday forefoot loading easier to manage.
Related forefoot conditions and how metatarsal support can fit in
In many people, forefoot overload sits alongside a more specific diagnosis, such as Morton’s neuroma, thinning of the fat pad, bunions, capsulitis at the lesser toes, sesamoiditis under the big‑toe joint, or marked arch changes. Each of the conditions below affects structures at or near the ball of the foot in a slightly different way, but all share a common theme: a small area under the front of the foot is being asked to do too much, too often, particularly during the push‑off phase of walking.
In each case, metatarsal support does not remove the underlying condition, but it can help by reducing local mechanical stress on sensitive tissues and improving how load is shared across the forefoot.
Using FootReviver Gel Cushion Ball of Foot Pads: fitting, comfort and care
How to put them on and position the gel
FootReviver Gel Cushion Ball of Foot Pads are designed to be worn directly against the skin. Each pad is built into a soft sleeve that slips over the front of the foot. There is a smaller sleeve for the big toe and a larger sleeve that sits around the other toes as a group.
The smaller sleeve comes part way up the big toe and provides gentle compression, creating a small amount of separation between the big toe and the other toes. The larger sleeve comes part way up the remaining toes together, lightly hugging them as a group rather than gripping each individual toe.
To put one on, sit down and slip the main part of the sleeve over the front of the foot so that the gel pad is on the underside. Gently slide the big toe into its own smaller sleeve so it feels lightly hugged, not pinched. Then slide the other toes together into the larger sleeve so that it sits part way up the toes as a group, with the front edge of the sleeve sitting behind the toe joints rather than over the ends of the toes.
The thickest part of the gel should sit under the ball of your foot – just behind the toe joints, roughly where a callus might form – rather than directly under the toe tips or far back in the arch. You should feel the main cushioning under the area where you push off, not under the ends of the toes or halfway along the foot.
The sleeve should feel snug but not painfully tight. If you want to wear socks, pull them on over the sleeve, not underneath it. Wearing a sock over the top helps keep the sleeve in place and reduces friction against the skin; if you try to wear the sleeve over a sock, the toe sleeves are more likely to twist or stretch and the pad may not line up properly under the ball of the foot.
Once the sleeve is in place, put your shoes on and walk a short distance on a familiar, level surface. If you mainly feel a lump directly under the toe tips, the pad is probably sitting too far forward and needs to be moved back slightly. If the front of the foot feels pulled tight and the pad feels closer to the arch than the ball of the foot, it may be too far back and needs to be eased forwards. Take a moment to adjust until the gel clearly feels centred under the ball of the foot without obvious bunching or tightness around the toes, and you can still move and spread your toes inside the shoe.
Getting used to wearing them
If you have not used metatarsal pads before, it is normal for them to feel different at first – typically a softer, slightly fuller feeling under the ball of your foot and a clearer sense that there is something under that area when you first start walking. As your feet adapt to the new way the pressure is spread, you usually become less aware of the pad itself.
It is often helpful to build up gradually. For the first few days, wear the pads for an hour or two at a time in shoes you already find comfortable, and on familiar routes. If that feels acceptable, you can then extend the time you wear them and include longer walks or more varied activities. Mild adaptation sensations, such as a stronger awareness of the pad or a slightly altered feeling under the toes, are common at the beginning and tend to settle as you get used to the support.
What you should not feel is a clear increase in sharp pain, new numbness, or strong pressure on the tips of the toes or the top of the foot. If that happens, it is worth checking the position of the pad and whether your shoes have enough space at the front. As a guide, you should still be able to move and spread your toes inside the shoe; if they feel cramped or pressed upwards, the combination of pad and footwear may be too tight.
Cleaning and maintenance
To keep the pads fresh and performing as intended, it is sensible to clean them from time to time. Hand‑wash them in lukewarm water with a small amount of mild soap, then rinse thoroughly. Gently squeeze out excess water without wringing or twisting, and allow them to air dry naturally away from direct heat sources such as radiators.
Machine washing or tumble drying is not recommended, as this can stretch or distort the elastic fabric and affect the shape and position of the gel pad. With sensible care, the sleeves are more likely to retain their fit and cushioning properties over repeated uses, so the way they support the ball of the foot remains consistent.
Safety and important information
Metatarsal pads can be a helpful way to make forefoot pain more manageable, but they are not suitable for every situation and they do not replace professional assessment where more serious problems may be present.
It is important to speak with a GP, podiatrist, or physiotherapist before relying on these pads as a main strategy if:
- You have diabetes, especially if you have reduced feeling in your feet or have been told you have neuropathy.
- You have significant deformity of the toes or forefoot, such as marked clawing, severe bunions, or a history of toe or forefoot fusion.
- You have had recent surgery in this area.
- You have known inflammatory joint disease affecting the feet, such as rheumatoid arthritis or gout, particularly if attacks are frequent.
You should not treat pads as the first thing to try, and should seek prompt medical advice instead, if you notice any of the following:
- Sudden, severe pain under the foot after an injury, especially if putting weight on the foot becomes very difficult or impossible.
- Marked swelling, redness, or warmth in the forefoot that is new or rapidly worsening.
- A very hot, red, exquisitely tender big‑toe joint that has flared quickly, which may suggest gout or infection.
- Changes in skin colour or temperature in the toes, such as going very pale, blue, or unusually cold compared with the other foot.
- New numbness, tingling, or loss of sensation under the foot that does not settle quickly.
- A suspicion that you might have a stress fracture or other bony injury – for example, pain that is very localised to one bone, consistently worsens with load, and does not improve with rest.
If the forefoot is very swollen, the sleeve may feel uncomfortably tight. In that situation, it is safer to reduce or avoid use until the swelling has been assessed and managed.
FootReviver Gel Cushion Ball of Foot Pads are designed as comfort aids to help modify local pressure under and just behind the ball of the foot. They are not medical devices for diagnosing, treating, curing, or preventing disease. People respond differently to any form of support, so experiences vary and no specific outcome can be guaranteed.
If you have persistent, severe, or rapidly changing symptoms; a history of diabetes with reduced foot sensation; significant foot deformity; recent forefoot surgery; or concerns about circulation or nerve function in your feet, it is sensible to ask a GP, podiatrist, or physiotherapist to assess things before you rely on these pads. If you are pregnant and develop new or rapidly worsening swelling or pain in the legs or feet, you should also seek medical advice promptly.
If you are unsure whether these pads are suitable for you, or if your pain does not improve or worsens despite using them, an assessment can help clarify what is driving your symptoms and what other options may be appropriate alongside or instead of metatarsal support.
30‑day money‑back guarantee
It is difficult to know in advance how a support will feel on your own feet, especially when comfort is so individual. To reduce that uncertainty, FootReviver Gel Cushion Ball of Foot Pads come with a 30‑day money‑back guarantee. This allows you to wear them in your usual footwear and day‑to‑day activities and to see how they feel over a reasonable period, rather than just during a brief try‑on.
Most people need a few days for their feet to get used to the changed pressure pattern before they can judge how much difference the pads make. The guarantee is there so that, after you have worn them consistently for a period of time, you have the option to return them within 30 days if they are not helping in the way you had hoped.
Recap: supporting the ball of the foot so walking feels more manageable
If the ball of your foot regularly feels bruised, burning, or as if you are stepping on a stone, it usually means a small area under the metatarsal heads is being asked to take more pressure than it can comfortably handle, step after step. Reduced natural cushioning, changes in the position of the metatarsal heads, irritation of the small nerves between them, and long periods on hard floors all make that pressure sharper and more frequent.
FootReviver Gel Cushion Ball of Foot Pads are designed around that mechanical problem. The built‑in gel pad sits under and just behind the ball of your foot, in the zone where pressure peaks at push‑off. It adds back cushioning over the plantar fat pad, supports the small arch across the ball of the foot so one or two metatarsals do not have to do all the work, and is held in place by the smaller sleeve for the big toe and the larger sleeve for the rest of your toes so it stays under the same part of your foot as you move.
These pads will not correct underlying deformities, remove a neuroma, or take the place of a proper assessment if your symptoms are severe or hard to explain. What they can do is reduce how sharply load is focused on sore points under the front of your foot and slow down how quickly pain builds when you are on your feet.
If the way your pain behaves matches what is described on this page, and your shoes have a little room at the front, it is reasonable to try FootReviver Gel Cushion Ball of Foot Pads and see whether they make long periods on hard surfaces and everyday time on your feet more tolerable. The 30‑day money‑back guarantee is there so you can make that decision based on how they feel on your own feet.
5 Reviews For This Product
Fast & Secure Checkout Through Paypal
Pay with Paypal the secure payment gateway that accepts all credit and debit cards. Paypal is free and secure and no credit or bank information is ever stored or shared with us.
Fast Dispatch
Enjoy your items soon with quick dispatch via Royal Mail. Expect to have your items between 1-3 working days for domestic orders. 7-10 Working days for international orders.
Return Policy – 30 Day Money Back Guarantee
In the unlikely event, you are unhappy with your purchase you can return it within 30 days for a refund. Please contact us via the form on the contact us page to start your return.
To return an item please send it to: Nuova Health UK, 81 Highfield Lane, Waverley, Rotherham, S60 8AL. Please include a note with your order id so we know who to refund. Please retain your postage receipt as proof of postage. All that we ask is that the item is in the original packaging and unused.











by Emma
I’ve been using them for a few weeks now, and I’ve noticed less pain. It’s like my feet are finally getting the care they need. If you’ve got Morton’s neuroma and you’re still on the fence, don’t hesitate, these pads are a worthy investment!
by Susan Young
Good pads work well.
by Amy
I’ve been dealing with Morton’s neuroma for a while, and boy, it’s been a struggle. The pain was like stepping on pebbles with each step. Now, I’m a waitress, standing all day and it was pretty much a nightmare. Then I got the Morton’s neuroma pads. They’ve been pretty amazing. Good comfort, nice fit in my everyday shoes, and they cushion my foot pretty well. The shock absorption is brilliant. The pain isn’t gone, but it’s manageable now.
by Cat Jones
I’m a nurse, always on my feet, and have battled foot discomfort for as long as I can remember. A colleague suggested these Morton’s neuroma pads. To be honest, I’m blown away with the relief they’ve given me.
They are super easy to use, the packaging was simple and straightforward, plus they fit nicely in my shoes. I love that they not just soothe pain, but they are designed to prevent my Morton’s neuroma from getting worse. I’ve noticed the difference, my feet are no longer throbbing by the end of my shift. I can’t recommend these enough! Personally, I feel like they’ve improved my work life because I’m no longer always stressing about my feet hurting.
by Janey
I got these pads for my mom who’s been suffering from the Morton’s neuroma for years. She’s always on the go, and the pain was getting to be too much. Now, she wears these pads under her feet every day, and she says it’s made a world of difference. She no longer feels the sharp, jarring pain with every step. It’s like these pads have given her her freedom back, and for that, we’re both incredibly grateful. Fantastic product, worth every penny!