No products in the cart.
Ankle Foot Orthosis Support Brace
£12.49inc VAT
- FootReviver™ semi‑rigid ankle foot orthosis brace for adults with painful or unstable ankles
- Available in Small (UK 3–5), Medium (UK 5–8) and Large (UK 8–11) and can be worn on either ankle
- Designed for recurrent ankle sprains, unstable ankles after injury, post‑fracture stiffness, tendon pain and ankle arthritis
- Rigid metal side splints rise just above the ankle bones to block sharp inward and outward rolls that cause “giving‑way”
- Open front and back let your ankle bend up and down so walking feels more natural than in a full boot or cast
- Cupped padded heel base cushions impact and helps keep the heel upright under the leg to improve alignment with each step
- Two wide adjustable straps pull the brace close for firm support and gentle, even compression around the ankle
- Soft, padded, moisture‑wicking lining and smooth seams reduce rubbing over bony or sensitive areas for day‑long wear
- Works best with roomier lace‑up trainers or walking shoes that can adjust around the brace
- Intended for everyday walking, standing and carefully building up activity once a clinician has said it is safe to load the ankle
- Start with shorter periods and higher‑risk activities such as uneven ground or stairs, then build up as tolerated
- Not suitable for fresh severe injuries, unstable fractures, or as a treatment or prevention for blood clots
- If your symptoms are severe, changing, or you are unsure, seek advice from a GP, physiotherapist or podiatrist before relying on this brace
Get 15% off - When bought together with:
- This item: Ankle Foot Orthosis Support Brace(£12.49inc VAT)
- Calf Support Compression Sleeves(£9.99inc VAT)
FootReviver™ Ankle Foot Orthosis Support Brace
Semi‑rigid side‑splint support for painful, unstable or recovering ankles
When you do not fully trust your ankle, simple movements start to feel like decisions you have to weigh up. You start thinking about which route feels safer, whether a set of stairs is worth the risk, or how far you feel comfortable walking before the ankle might “go” again.
You might find yourself placing each step carefully on uneven paths or grass because you are worried the ankle might roll. You may slow right down on stairs, especially going down, because the ankle bends and twists more and feels vulnerable. A sharp pull or ache around the ankle or back of the heel may appear when you push off to walk faster or climb a slope or ramp. By the end of a long day on your feet, you might notice a deep throb, swelling or stiffness around the ankle.
It can be draining when such ordinary movements start to feel like something you have to plan around. These changes are common after repeated ankle sprains where ligaments were stretched or partly torn and never fully rehabilitated; after time in a cast or walking boot for a fracture or surgery, leaving the joint stiff and muscles weak; with tendon problems around the ankle and heel, such as Achilles pain, where tissues dislike repeated strong pushes and sharply bent positions; and with long‑standing ankle arthritis or wear‑and‑tear, where the joint surfaces are already sensitive to twisting and load.
In all of these situations, the joint struggles most in certain positions: when the ankle rolls in or out sharply, straining the ligaments and tendons on that side; when the heel tilts too far towards the inside or outside so forces pass unevenly through the back of the foot; and when the ankle is pushed to the very end of its bend or twist so joint surfaces are pressed hard together.
Those positions place extra strain on ligaments, tendons and already‑irritated joint surfaces. When the same sharp roll, twist or fully bent position is repeated through the day – stepping off kerbs, turning on narrow landings, walking on sloping pavements – symptoms are easily re‑triggered just as you feel you are improving.
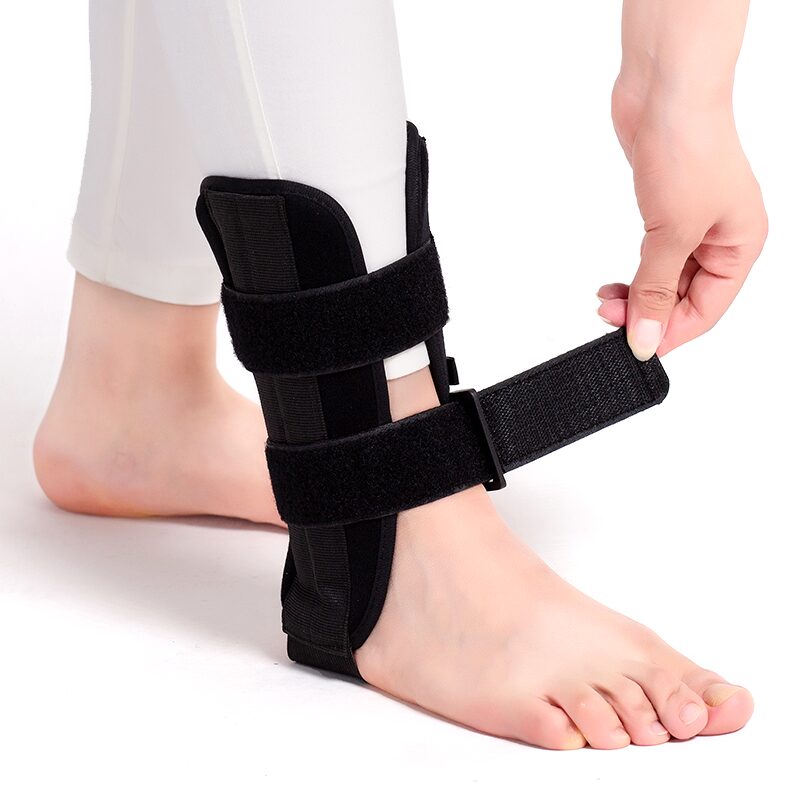
The FootReviver™ Ankle Foot Orthosis Support Brace is a semi‑rigid support for people with these kinds of ongoing or recovering ankle problems. It combines rigid metal side splints along the inner and outer ankle to resist excessive rolling, a cupped padded heel base to cushion impact and guide the heel into a steadier position, and wide adjustable straps around the lower leg and ankle to keep everything close and supported. Together they limit the uncontrolled rolling and twisting that tend to provoke pain and “giving‑way”, while still allowing the ankle to bend up and down so you can walk and manage many daily tasks. It is not designed for fresh, severe injuries that may need urgent medical assessment or full immobilisation.
Why your ankle keeps flaring – and what is happening inside it
Many people with ankle pain or instability find it comes and goes. Some days feel almost normal, others are worse, and certain activities – a twist on uneven ground, a long day on hard floors, more stairs than usual – reliably bring symptoms back.
To understand why, it helps to look at the main structures involved.
The ankle joint sits where the shin bone meets the ankle bone, with the heel bone directly underneath. These joints allow the foot to point up and down and make small side‑to‑side adjustments as you walk. Problems here are often felt as a deep ache or sharp catch around the front or sides of the ankle, sometimes with a “jammed” feeling at the end of movement.
Ligaments are strong bands connecting bone to bone. Around the ankle they act like check‑straps, stopping the joint rolling or twisting too far. When they are overstretched or torn, they can remain slightly lengthened as they heal, so they do not pull up as firmly as before. This can leave you with tenderness around the inner or outer ankle and a recurring sense that the joint might suddenly give way.
Tendons connect muscles to bone and act like the body’s internal cables. Around the ankle and heel they have to transmit force every time you push off, change direction or balance. They are generally happiest with steady, repeated work and dislike sudden jumps in how much work they have to do, very strong pushes, or being pulled round sharp corners. When irritated, they often hurt most with movement or load – on slopes, stairs, or when you push off – and can feel stiff or “creaky” after rest.
The joint capsule and surrounding soft tissues wrap around the joint to help contain fluid and guide movement. When inflamed or thickened, they contribute to aching, swelling and a sense of tightness, especially at the ends of movement.
Here, “load” simply means the amount of force or work these structures have to handle – how much body weight they support, how hard they are pulled, and how often during the day. When any of these tissues are injured, overloaded or worn, they tend to be irritated by particular movements and loads. The same movements, repeated day after day – a repeated small roll of the ankle, standing long hours on hard ground, frequent twisting and turning – can keep problems simmering because tissues are stressed again before they have had time to calm down properly. Over time, their tolerance drops, and flare‑ups arrive with smaller triggers.
The FootReviver™ brace is mainly used for four situations: recurrent sprains and long‑standing “giving‑way”; the period after a fracture or immobilisation; tendon pain around the ankle and heel; and ankle arthritis with long‑standing joint wear. All four share a common problem: the ankle or heel is not coping well when it twists or rolls under load, and sometimes also when it is asked to take heavier or more sudden loading at certain angles. The brace is designed to limit those specific movements while still allowing useful up‑and‑down motion.
Recurrent ankle sprains and ankles that keep “giving way”
Many people can remember the exact moment of a significant ankle sprain: stepping off a kerb and rolling the ankle inwards, landing awkwardly from a jump, or twisting on an uneven surface. The foot usually rolls in (inversion) and the ligaments on the outer side are forced beyond their safe range.
After the initial swelling and bruising settle, ongoing problems often include local tenderness at the outer side of the ankle, especially when pressing over the ligaments; vague or sharp discomfort and mild swelling after walking on rough or sloping ground; a sense that the ankle might give way if you move quickly or step on something unexpected; and feeling “shaky” or cautious on that ankle, even on better days, with occasional “almost went over” sensations.
Inside the joint, the outer ligaments have been partly torn or overstretched. As they heal, they may remain slightly lengthened, so they no longer check movement as firmly as they once did. The small nerve endings within those ligaments that tell the brain where the joint is can also be disrupted, so messages about ankle position arrive slightly slower or less clearly than before.
As a result, when your foot starts to roll inwards, there is less early resistance from the ligaments and your muscles are slower to realise what is happening. The ankle can tip further before protective muscles pull you back. You experience this as the ankle suddenly lurching or “nearly going” even on modest uneven patches. This is why a shallow dip in the pavement or a small stone underfoot can feel like a much bigger “turn”.
Over time, each small give‑way can stretch healing fibres a little again, and repeated small extra stretches can gradually lengthen the ligaments further. Chronic ankle instability – what many people call an “unstable ankle” – can develop, with a persistent feeling of looseness, occasional sharp twinges, and a tendency to avoid quick changes of direction or uneven ground. On good days, pain may be low, but those altered position signals and laxer ligaments are still there, so the risk of another “turn” remains.
A brace that physically resists the ankle rolling too far, and slows any roll that does begin, can reduce how often you reach those vulnerable positions while you work on strength and balance exercises to improve your own control. The FootReviver™ splints are set to rise just above the ankle bones so they meet that inwards or outwards roll early and limit how far it can go.
After a fracture or time in a cast or boot
When a bone in or around the ankle has been broken, a cast or rigid boot is often used to hold everything still while the bone knits. This protects the fracture, but it also means that the surrounding muscles, ligaments and cartilage do very little for several weeks.
Once the cast or boot comes off, many people notice pronounced stiffness when they first try to bend the ankle up or down, as if something is blocking the movement. Weakness and a “wobbly” feeling around the ankle and calf are common, especially when trying to stand on that leg alone. Even a small roll or twist can feel dramatic, and there may be a lack of confidence in placing weight through that leg, particularly on uneven ground or slopes.
During immobilisation, the muscles that help stabilise and move the ankle, especially the calf and the small muscles around the shin and foot, have been used far less, so they are weaker and fatigue more quickly. Ligaments and the joint capsule have had very limited movement, so they become less stretchy and less able to accommodate sudden changes. Joint surfaces and cartilage have taken less everyday load, so when normal forces return they can feel unusually sensitive.
When you start to move again, the bone may be strong enough to take weight, but the tissues that should control the ankle are not yet ready for sudden twists or unpredictable surfaces. Your usual balance reactions are out of practice; even a minor wobble can feel much larger than it is.
Without planned rehabilitation, some people avoid using the ankle properly, keeping most of their weight off that side. This can lead to ongoing stiffness, weakness and a persistent limp. Others use pain alone as a guide and push too fast, risking a sudden twist or overload before ligaments and muscles have regained enough control.
A typical rehabilitation plan after immobilisation involves a gradual increase in weight‑bearing, movement and strength work. Alongside this, limiting large rolls and twists while still allowing controlled up‑and‑down movement lets the bone, joint surfaces and soft tissues adapt back to normal life without being pushed into the positions that most often set symptoms off. A semi‑rigid brace like FootReviver™ can be useful here: it lets you practise walking, standing and using stairs with additional sideways control, rather than asking an ankle that has been rested for weeks to cope with all the demands of walking and stairs on its own. Clinicians often look for this type of brace once a cast or boot has been removed and you are cleared to start moving more, but do not yet feel safe on uneven ground.
Tendon pain around the ankle and heel (including Achilles)
Tendons around the ankle and heel are heavily involved in walking, climbing stairs and balancing. When they become irritated, how they feel is different from a sprain or fracture.
People with tendon‑related ankle or heel pain often report a sharp or aching pain at the back of the heel or just above it, especially when walking up or down slopes, climbing stairs or pushing off to walk faster. Others feel an aching or pulling along the inner side of the ankle and arch after longer walks or standing, sometimes alongside a flattening arch. There may be tenderness or catching along the outer side of the ankle behind the bony lump, particularly after sideways movements. Stiffness after rest, such as first thing in the morning, that eases slightly with gentle movement but can build again with heavier use later in the day is also common.
Key tendons include the Achilles tendon at the back of the heel, linking the calf muscles to the heel bone and coping with high forces every time you push off the ground; the posterior tibial tendon on the inside of the ankle, which helps support the arch and control inward rolling of the heel; and the peroneal tendons on the outer side of the ankle, which help prevent the foot rolling inwards too far and assist with side‑to‑side control.
Tendons are built to handle repeated work, but they cope poorly when there is a sudden jump in how much work they have to do, such as a sharp rise in walking or running over a short period; when they are loaded for long periods at awkward angles – for example if the heel persistently tilts inwards or outwards so the tendon curves tightly around a bone; or when they are repeatedly taken towards the very end of their length under tension, such as in deep ankle bends or forceful push‑offs.
Inside the tendon, the tough collagen fibres that usually sit in neat, parallel bundles can become disorganised and thickened in small areas. This makes that region less efficient at handling pull, stiffer after rest, and more easily irritated when forces rise quickly.
This is why tendon pain often feels stiff and sore with the first steps after rest – the fibre bundles and surrounding tissues are not yet gliding smoothly – then eases somewhat as you move around and blood flow and temperature increase, before flaring again if you keep loading it hard in challenging positions, particularly on slopes, stairs or uneven ground later in the day. The pain you feel first thing is linked to irritation built up from earlier loading; supports like braces are most useful in changing what happens from that point onwards, not during sleep.
For example, walking uphill or downstairs bends the ankle upwards more and lengthens the Achilles under load. If, at the same time, the heel is dropping and tilting inwards, one part of the tendon is being stretched and compressed more than usual and can be quite painful with each step. If the heel repeatedly rolls inwards, the posterior tibial tendon on the inside of the ankle has to work harder, for longer, to slow that roll and support the arch. After a day of standing or walking on hard floors, it may feel hot, aching and tender.
Because these tendons are strongly influenced by heel and ankle position, controlling side‑to‑side roll and reducing extreme heel tilt can help calm them. The goal is not to remove all load – tendons need a certain amount of work to recover – but to avoid the repeated sharp angles and surprise pulls that keep flaring symptoms. A brace that helps keep the heel nearer upright and moderates sudden rolls can make it easier to build the right kind of strength and conditioning programme around that tendon. If how the tendon is loaded stays the same and it is taken back to its sore end of movement day after day, irritation can drag on for many months and flares may appear with smaller triggers over time.
That is why for many people with tendon‑related ankle or heel pain, extra control at the heel – rather than complete rest – is a key part of getting back to steadier walking.
Ankle arthritis and long‑standing joint wear
Ankle arthritis develops when the smooth cartilage that lines the joint surfaces becomes thinner, rougher or damaged. This may follow earlier injuries such as fractures or severe sprains, or develop gradually when the joint has been exposed to long‑term mechanical stress. It is generally less common than arthritis in the knee or hip and is often linked to previous ankle trauma.
People with ankle arthritis typically notice a deep, aching pain around the front or sides of the ankle, especially after walking or standing on hard surfaces. Stiffness when starting to move, for example after sitting for a while or first thing in the morning, which eases as the joint “warms up”, is common. Sharp twinges can occur with sudden twists or when the ankle is pushed to the end of its range of motion. Swelling or a sense of fullness around the joint often appears after heavier use.
Thinner cartilage means less cushioning between the bones, so load is transmitted more directly to the underlying bone, which can become irritable. The joint capsule and surrounding tissues may become thickened and less flexible, which can further reduce movement and contribute to stiffness. The joint usually tolerates movement best in a comfortable middle part of its movement, where the foot is roughly at right angles to the shin, not bent fully up or fully down. It tends to react badly to positions at the very end of its bend or twist – deep bends, full twists and sharp pivots – and to large, uneven loads.
This is why someone with ankle arthritis might find a short walk on level ground manageable but struggle more on uneven paths, slopes or with sudden changes in direction, and find that standing for long periods on hard flooring gradually increases aching and swelling.
Over time, if the joint is repeatedly pushed into the same aggravating movements, the irritated capsule and tissues around it can thicken further and lose more flexibility. Pain may start earlier in the day or with shorter walks than before, and everyday activities can become more restricted.
Keeping the ankle moving gently within its comfortable middle range usually helps, because it aids joint lubrication and can reduce stiffness. Supporting and guiding the ankle so it spends more time in that range, and less time in sudden, extreme positions, can make daily movement more manageable, even though it does not change the underlying cartilage wear.
Across recurrent sprains, post‑fracture stiffness, tendon problems and arthritis, the same issues with how the ankle moves keep appearing: an ankle that is unhappy when rolled or twisted sharply, a heel that tips too far in or out, and sensitive tissues that react badly when they are pushed to the very end of their movement under load.
A semi‑rigid ankle‑foot brace is designed to limit those particular motions and loads, while allowing enough natural movement for walking and recovery. FootReviver™ is intended to sit alongside exercises, appropriate activity levels and suitable footwear, not replace them.
How the FootReviver™ brace is built for these ankle problems
The FootReviver™ brace is not intended to lock the ankle completely. Instead, it is built to:
- firmly restrict movements that most often cause damage or provoke pain, particularly side‑to‑side rolling and extreme tilting; allow controlled up‑and‑down bending so you can walk and carry out daily tasks; support the heel and ankle in a more neutral, repeatable position; and provide adjustable, comfortable support during the times when your ankle is under most strain.
- Rigid metal side splints mainly tackle the excessive roll described above. The open front and back allow the ankle to bend for walking. The cupped padded heel base helps with heel position and impact. Wide straps bring everything close to the limb and allow you to set the level of support. Each part of the brace has a specific job.
- Soft elastic sleeves around the ankle mainly give gentle compression and awareness. Full rigid boots aim to stop almost all ankle movement. FootReviver™ sits between these: it allows you to bend the ankle for walking while firmly limiting the sharp rolls that usually cause trouble for unstable or arthritic ankles.
Rigid side splints – controlling the roll that drives sprains and tendon flare‑ups
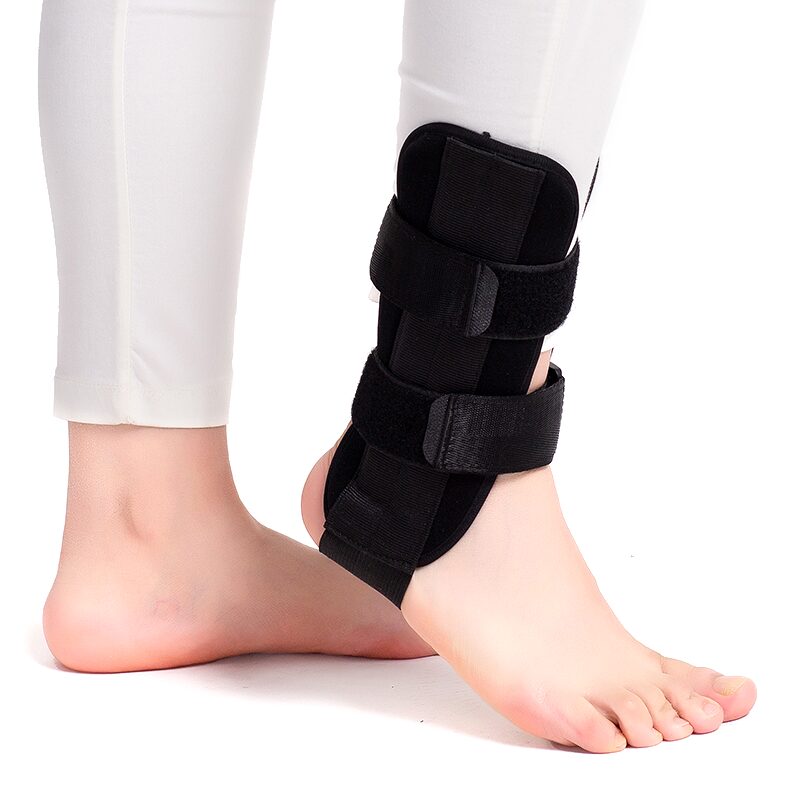
Two rigid metal splints are built into panels on the inner and outer sides of the FootReviver™ brace. They run up the sides of the lower leg and ankle, extending just above the ankle bones. For them to work properly, they need to sit alongside those bony points rather than rotated forwards or backwards.
These splints resist inversion (rolling inwards) and eversion (rolling outwards) beyond a safer range, help keep the heel more upright under the leg rather than tilting sharply to one side, and slow down any roll or twist that does occur, giving your muscles a better chance to react before the ankle reaches its sore end‑position.
In recurrent sprains and chronic instability, the outer ligaments no longer have to work alone to prevent the ankle dropping into inversion. The splint on the outer side acts as a firm physical block if the foot starts to roll inwards. When you land on a slightly uneven paving slab, the splint meets that roll earlier and reduces how far the ankle can tip, so the overstretched ligaments are not dragged to the very end of their range every time. Because the splints slow the speed of any roll, the small position‑sensing nerves and supporting muscles have a fraction more time to detect and correct the movement, which can help reduce those sudden “almost went over” moments and gradually rebuild confidence.
In tendon problems, the peroneal tendons on the outer side are less often pulled round the outer ankle bone in a tight curve, because the ankle cannot roll as far inwards. When you walk on slopes or turn, the splint limits the sharpest part of that roll, which may reduce the intensity of the pull on these tendons. The posterior tibial tendon on the inner ankle is under less constant tension from a collapsing inward heel, as the splints help keep the heel closer to an upright position under the shin. During longer spells of standing, it is not continually fighting against your heel dropping in.
In ankle arthritis, reducing side‑to‑side sway and sudden twists lowers the sliding forces between the joint surfaces. Instead of repeatedly loading the same small, sore patch of cartilage during each sharp roll, the joint is kept closer to the part of its movement where forces can be spread more evenly as you walk and stand.
Open front and back – allowing controlled bending for more natural walking
There is no rigid panel across the front of the ankle or directly behind the Achilles tendon. The FootReviver™ brace is open in these areas, with the side panels connected by padded material and straps.
This allows the ankle joint to bend upwards as the body moves over the foot during walking or when going downstairs, and to point downwards when pushing off the toes, climbing stairs or standing on tiptoe, within a comfortable range.
This means that after sprains and fractures, the ankle and surrounding soft tissues can move enough to regain flexibility and strength, rather than being held rigid for longer than necessary. Tendons such as the Achilles can move through a useful middle part of their movement so they warm up with gentle movement, instead of feeling locked and then suddenly loaded. In arthritis, the joint can keep the gentle motion that is usually more comfortable than being fixed still.
Compared with a full rigid boot, this semi‑rigid design offers less protection against all movement but more practicality and more natural walking once tissues are ready for it. By allowing up‑and‑down bending while still restricting side‑to‑side roll, the FootReviver™ brace aims to support safer walking mechanics in the later stages of recovery, such as when you first return to walking reasonable distances or using a full flight of stairs; let muscles and tendons continue to work, helping stability and circulation; and avoid forcing all movement into the knee or hip by locking the ankle completely during everyday tasks.
Cupped heel pad – supporting the back of the foot where forces start
Under the heel, a padded, slightly cupped section connects the two side panels. It acts as both a cushioning base and a gentle guide for heel position.
This heel section cushions impact directly under the heel bone, which can be tender in tendon problems, arthritis, plantar heel pain or after impact injuries. It encourages the heel to sit between the side splints rather than collapsing to one side, and it helps keep the heel bone tilted less towards the inside or outside as you place weight through the leg.
This is particularly relevant to what was described earlier. In posterior tibial tendon problems and plantar heel pain, an inward‑tilting heel increases tension along the inner ankle and arch. The heel pad and splints together limit that tilt, reducing repeated strain along the inner edge of the foot when you stand on hard floors or walk for longer periods. In outer‑ankle tendon issues and pain along the outer border of the foot, excessive rolling onto that outer edge can aggravate symptoms. Keeping the heel nearer upright means weight is spread more evenly across the heel and midfoot with each step, rather than repeatedly driving into the sore outer strip.
In arthritis, a more stable heel position reduces sudden shifts in force across already‑sensitive joint surfaces. As you walk along slightly sloping ground, the guided heel position helps stop all your weight from being channelled into the most irritable part of the joint on every step.
In everyday walking, the heel is usually the first part of the foot to make contact with the floor. Improving heel position at that moment can influence both the direction and spread of forces up through the ankle with each step, and for some people, this helps reduce the severity of sudden sharp pains or end‑of‑day aching linked to repeated poor heel alignment.
Wide adjustable straps – setting support and compression to match your day
Two wide elastic straps sit around the lower leg and upper ankle, above the heel. Each passes through a buckle and folds back, allowing you to vary the tension.
These straps pull the side panels in towards the leg so that the splints and padding stay in close, consistent contact with the ankle. They wrap around the back of the lower leg, including the Achilles region, and across the front of the ankle, giving support around the joint. They also provide adjustable compression around the ankle area.
Many of the problems described earlier produce swelling towards the end of the day, especially after sprains, fractures or arthritis flares. Mild, even compression can help by gently supporting soft tissues and limiting how much fluid collects. The straps allow you to set a firmer level of support when you expect more demand, such as a longer walk on varied surfaces or a day when you will be on your feet more than usual; ease the tension slightly at times when the ankle feels more settled, while still keeping the brace in place; and make small adjustments during the day if the ankle swells or settles.
Compression should never be so strong that it causes numbness, tingling, marked colour change or throbbing in the toes or foot. Over‑tight strapping can itself irritate nerves and blood vessels and make discomfort worse. The aim is a supportive “hug” around the joint, not a tourniquet. If you have known circulation or nerve issues, it is particularly important to use moderate tension and follow professional advice. The adjustability helps you find and maintain that middle ground as your ankle’s behaviour changes through the day.
Soft lining and smooth seams for day‑long comfort
The inside of the FootReviver™ brace is lined with soft, padded material designed to sit comfortably against the ankle and lower leg, with extra cushioning over bony points such as the ankle bones, a fabric surface that helps draw moisture away from the skin, and smooth, rounded edges and flatter seams placed away from common rubbing spots.
Rigid or semi‑rigid supports that press directly on bare skin can quickly become uncomfortable, particularly over bony areas. If a brace causes rubbing, blisters or skin irritation, people tend to remove it just when they start to tire or move more carelessly – the very time when stability is most needed. As people get older or if they live with certain long‑term conditions, skin often becomes thinner and more fragile, so minimising friction is especially important.
Being able to wear the brace for the times of day when your ankle does the most work – such as longer walks, days when you are on your feet more, or dealing with uneven ground – is crucial for it to provide enough extra stability for you to notice a difference. Comfort is therefore part of what makes consistent use possible, not an afterthought.
Getting the right size, fit and footwear with FootReviver™
The FootReviver™ brace is designed for adults and comes in three approximate size ranges based on UK shoe size: Small (3–5), Medium (5–8) and Large (8–11). It can be worn on either the left or right foot and is suitable for both men and women.
A correct size and good fit ensure that the side splints sit alongside the ankle joint, not too far up the leg or down onto the foot; the heel is positioned on the cupped heel pad so cushioning and guidance occur where intended; and the straps can be tightened enough to stabilise the brace without digging in or over‑compressing the leg.
Shoe size is a guide. If your ankle and lower leg are particularly slim or broad for your shoe size, check that the brace does not gape away from the leg when the straps are reasonably tight, that it does not spin or slide when you walk, and that you are not having to pull the straps to their absolute limit and still feeling loose.
Because the brace adds some bulk around the sides of the ankle, it typically works best with roomier footwear, such as lace‑up trainers or walking shoes that can be loosened then adjusted over the brace and that have more depth around the ankle. Very tight or narrow shoes are unlikely to accommodate it comfortably and may interfere with its positioning. Relatively flat, supportive shoes are usually more compatible than high‑heeled or very minimal designs.
Many people find it helpful to have at least one pair of shoes that they know works well with the brace, so they are not forced to choose between adequate support and shoes that feel too tight.
The brace can also be worn without footwear indoors, for example when moving around the home. In that case, take extra care on smooth surfaces such as tiles or polished floors, and be particularly cautious on stairs.
A thin sock worn under the brace often strikes a good balance between comfort and control. Very thick socks can change how the brace grips the leg and may reduce its stabilising effect.
What level of support FootReviver™ gives – and when people usually use it
This is a semi‑rigid support. In practical terms, it offers more control than a soft elastic sleeve, which mainly provides gentle compression and awareness of the joint, and it is less restrictive than a full immobilising boot or cast, which aim to stop almost all ankle movement.
It is generally intended for people whose ankles need firm sideways guidance and support during everyday activities; can bend up and down but feel vulnerable or painful with uncontrolled roll or twist; and are past the very early, unstable fracture stage where complete immobilisation is often required.
People tend to find this level of support helpful for everyday walking on pavements or paths where you cannot fully predict the surface; standing for moderate periods, such as days that involve more time on your feet; and carefully returning to lower‑impact exercise, such as brisk walking or controlled indoor exercise under professional advice, where side‑to‑side control is particularly important.
It is not a first‑line treatment for fresh, unstable fractures or severe acute injuries, which usually require immediate medical care and often more rigid immobilisation. It is not designed for use in water, and it is not a guarantee of safety in higher‑impact or contact activities, where individual clinical guidance and sometimes additional protections are needed.
Understanding what the FootReviver™ brace can and cannot do helps keep expectations realistic. It is intended to reduce specific unwanted movements – especially rolling and sudden twists – and to support the ankle during daily movement. It does not hold the joint perfectly rigid, eliminate all pain, or replace the need for rehabilitation and attention to how you walk and stand.
Who this brace is most suitable for – and who should seek advice first
This brace is designed for adult ankles that need firm guidance and stability but are not in need of full immobilisation. It is mainly aimed at joint, ligament and tendon problems rather than primary nerve conditions, unless a clinician has advised otherwise.
It is most likely to help people with recurrent sprains or chronic instability. If you recognise the experience of repeatedly “going over” on the same ankle, feeling unsteady on uneven ground, or hesitating on stairs because you do not trust the joint, this level of side‑to‑side control is often appropriate. Using a semi‑rigid brace for situations you already know tend to set your ankle off, such as uneven pavements or longer flights of stairs, can reduce the chance of further sprains by blocking the more extreme inward and outward rolls described earlier, while you work on strength and balance exercises to improve long‑term control.
It is also suited to people moving on from a cast or boot after an ankle‑related fracture or surgery, once a doctor or physiotherapist has confirmed that the bone has healed enough for more movement and weight‑bearing. A semi‑rigid brace can support the transition back to walking by helping to prevent uncontrolled twists while muscles and ligaments regain strength and range. For many people, this is a temporary stage rather than a permanent need. As your own control improves through rehabilitation exercises, you and your clinician can decide when to rely less on external support.
People with tendon‑related ankle and heel problems may also benefit. If pain tends to occur at the back of the heel or around the inner or outer ankle when walking, especially on slopes, uneven ground or with faster walking, and you have been told that a tendon is involved, controlling heel tilt and side‑to‑side motion can be part of a sensible plan. By keeping the heel nearer upright and slowing sudden rolls, the brace may reduce how often the tendon is pulled into its sore end of movement while you rebuild strength and tolerance with exercises. If you recognise this picture but have not had a specific diagnosis, it is worth discussing it with a clinician first.
People with ankle arthritis may find that when deep ankle ache, stiffness and twinges with small twists limit walking or standing, extra stability helps keep the joint closer to its more comfortable middle part of movement during everyday activities. The aim is to support you to stay as active as is comfortable by reducing sudden, sharp twists and jolts at the very end of movement, not to immobilise the joint completely or change the underlying cartilage wear.
Before using this brace, or any similar support, seek professional advice promptly if you have a new injury with severe pain, significant deformity or immediate inability to bear weight; suspect a fracture or significant ligament rupture; have very fragile skin, known serious circulation problems, or long‑standing deformity of the ankle or foot; or notice symptoms that might indicate a blood clot, such as unexplained calf pain or tenderness, one leg becoming more swollen than the other, warmth and redness, or sudden shortness of breath.
This brace does not treat, reduce, or prevent blood clots, deep vein thrombosis, or similar conditions. If you are at increased risk of clots, or have recently had a leg injury or period of immobilisation, it is essential to follow the guidance of your GP or specialist about movement, medication and monitoring. Remaining sensibly active as advised is usually important for circulation, and no external support should be relied upon to replace that.
If your symptoms do not clearly match what is described here, or are more complex, it is sensible to have them assessed before relying on a brace. A GP, physiotherapist or podiatrist can help you decide whether this form of support is appropriate and how best to integrate it into the plan you have agreed together.
How to use this brace in daily life
Once you know that a brace of this type is suitable for you, how you use it day to day makes a real difference to how effective it can be.
Most people get the most benefit from wearing it for activities and times when the ankle is under more strain, such as longer walks, uneven ground or busier days; introducing it gradually rather than wearing it continuously from day one; and combining its use with exercises and movement strategies recommended by a clinician.
Fitting the brace
The aim is to position the brace so that your heel sits centrally on the padded heel section; the rigid splints lie along the inner and outer sides of your lower leg and ankle, roughly over the ankle bones; and the brace hugs the ankle and lower leg without twisting or gaping.
When you put it on, place your heel on the heel pad so that it neither hangs over the back edge nor sits too far forwards. Align the side panels so the stiffer sections sit directly over the sides of the ankle, not rotated towards the front or back. A quick check is that the splints run roughly over the bony bumps at your ankle. Thread each wide strap through its buckle and fold it back, pulling gently until the brace feels firm but still comfortable.
A thin sock worn under the brace can help reduce friction and absorb sweat, especially if you plan to wear it for longer stretches. Very thick socks can change the way the brace grips your leg and may reduce how effectively the splints control roll. On the first few uses, it is sensible to check the skin under the brace after removing it, to make sure there are no areas of rubbing or pressure, especially if you have reduced sensation or more delicate skin.
Once fitted, you can either put a suitable, roomier shoe over the top for outdoor walking or work, or wear the brace without footwear indoors, provided the floor surfaces are not slippery and you take particular care on stairs.
Adjusting strap tension
The two wide straps give you control over how much support and compression you apply.
A sensible approach is to start with moderate tension so the brace feels stable but not restrictive. Walk a short distance and notice whether the ankle feels well held or loose inside the brace. If it feels loose, you can tighten the straps a little. If you notice any numbness, tingling, unusual colour change or throbbing in the foot or toes, loosen the straps straight away.
During the day, you may choose to tighten the straps slightly before activities that you know challenge your ankle, such as walking on uneven paths, doing more stairs or standing for longer. As the ankle fatigues or swells, small adjustments can help maintain a comfortable level of support. On days when you are doing less, you can wear the brace more loosely while still benefiting from the guidance of the splints and heel support.
If you repeatedly find you have to tighten the straps much more than when the brace was new to get the same sense of support, it may be a sign that the elastic has worn or the fit is not ideal. In that case, it is worth discussing this with a clinician or retailer.
The key is to find a balance where the ankle feels held and supported, but you can still move comfortably and your foot feels normal in terms of sensation and temperature.
Building up wear time
Most people benefit from introducing the brace gradually rather than wearing it continuously from the outset.
One sensible way to start is to use the brace for specific activities where your ankle usually feels most vulnerable – for example, going outside for a walk or tackling a set of stairs – for around 30–60 minutes at a time, depending on comfort. As you adjust to the feel of the brace and your ankle tolerates this, you can extend these periods and add further situations, such as parts of your day that involve more walking or standing. With help from your clinician, you can then decide whether the brace is best used daily for a while, or mainly for higher‑risk days and activities as your confidence and control improve.
These timings are guides rather than strict rules. Some people will need shorter or longer periods. The brace is generally not used for sleeping unless a clinician has specifically advised this. It often works best when wear‑time is increased alongside a planned exercise programme that builds your own muscle strength and balance, so over time you depend less on external support.
Using it with footwear and on different surfaces
Because this brace adds some bulk around the ankle, lace‑up trainers or walking shoes that can be loosened and then retightened around the brace tend to work best. Shoes that are already snug around the ankle and top of the foot may not be practical to combine with this design. Relatively flat, supportive shoes usually help the brace work as intended.
Indoors on flat floors, some people with milder or later stages of recovery choose to move carefully without support for short periods and use the brace when tackling stairs or carrying items. Outdoors, especially on uneven pavements, grass, gravel or sloping paths, many people appreciate the extra stability the brace provides. For any return to exercise, it is important to follow your clinician’s advice, as needs vary widely depending on the type of activity and stage of recovery. The brace can help with side‑to‑side control but does not remove the need to build activity up gradually.
The brace is not designed for use in water and should be removed for bathing or swimming.
What to expect over time
With regular, sensible use, many people find that the ankle feels more secure in the specific situations that used to provoke giving‑way, such as stepping off small drops or walking over uneven ground. Sharp pains triggered by sudden rolls or tilts are often less frequent when the brace is on, and swelling and aching at the end of busier days can feel more manageable.
The brace does not change the internal structure of tendons, ligaments or cartilage. What it can do is change how often those tissues are pushed into positions that you already know cause trouble. By reducing exposure to extreme positions and sudden twists that repeatedly irritate sensitive ligaments, tendons and joint surfaces, it can make it easier and safer to work on strength, balance and movement patterns, often with exercises prescribed by a clinician, and support daily movement while other aspects of treatment and self‑management take effect.
If, despite appropriate use, pain or instability are getting worse, or new symptoms appear, it is important to seek further assessment rather than simply increasing the amount of time you wear the brace.
Safety: when to pause and seek professional advice
A brace like this can be a helpful option, but it is not a substitute for medical assessment when certain signs are present.
You should seek advice from a GP, physiotherapist, podiatrist or urgent care service if you have a new injury with severe pain, obvious deformity, or cannot put any weight on the leg. A high‑energy injury, a clear change in the shape of the ankle, or severe pain with any attempt to stand can indicate a fracture or major ligament injury that needs urgent imaging and assessment.
You should also seek advice if pain, swelling or bruising are rapidly worsening over hours or a few days, rather than following the more typical pattern of swelling that slowly settles. This may indicate complications that need a clinician’s review.
Changes in skin colour or temperature below the brace, such as new redness, paleness, or an unusually cool or hot sensation compared to the other side, may be a sign of circulation or inflammatory problems, especially if combined with pain. New numbness, tingling or weakness in the foot or toes can be related to nerve involvement or pressure and should not be ignored, particularly if they occur even when the straps are not overly tight.
If you are worried about a possible blood clot, with symptoms such as unexplained calf pain or tenderness, one leg becoming more swollen than the other, warmth and redness, or sudden shortness of breath, this should be treated as urgent and assessed the same day.
This ankle‑foot brace does not treat, reduce, or prevent blood clots, deep vein thrombosis, or similar conditions. No external support should ever be relied on for that purpose. If you have already been advised that you are at increased clot risk, it is important to follow specific recommendations about movement, medication and monitoring. If any of the warning signs above appear, they should be taken seriously whether or not you are wearing a brace.
More generally, if ankle or foot symptoms are persistent, clearly worsening, or change in pattern, severity or location, they should be reviewed with a healthcare professional. A brace is not a diagnostic tool and should not be used to delay appropriate investigation. Advice on diagnosis, imaging and broader treatment options – including whether to continue, change or stop using a brace – is best given by someone who can examine you in person and consider your full medical history.
If you are in doubt, it is safer to have your ankle or foot checked than to carry on and hope it will settle on its own.
Other ankle and foot problems where FootReviver™ may help
Some foot and ankle problems are less central to the FootReviver™ brace but share similar ways the ankle and heel are being loaded and twisted. For some people, this brace may contribute to their management alongside other measures.
Looking after your FootReviver™ brace and how long it should stay supportive
Cleaning and drying
For this type of padded brace, hand‑washing is recommended. Undo the straps so the interior is exposed. Wash the brace in lukewarm water with a small amount of mild detergent, avoiding bleach or harsh chemicals. Rinse thoroughly to remove any soap residue. Gently squeeze out excess water without twisting or wringing it. Allow it to air‑dry naturally at room temperature, away from direct heat sources and strong direct sunlight.
Letting the brace dry fully between uses helps keep the lining fresher and more comfortable against the skin.
How often to wash depends on how frequently and how long you wear it, and how much you sweat. As a rough guide, washing once or twice a week often works for regular use. If you wear it for long periods or in hot weather, you may want to wash it more often if odour or skin comfort become an issue. The aim is to keep the brace pleasant to wear rather than to follow a strict washing schedule.
How long your brace is likely to stay supportive
With regular adult use, the rigid side splints are designed to retain their shape and supporting role over many months. Padding and fabric may compress slightly over time, which is normal. The elastic straps will gradually lose some tension after repeated tightening and loosening, as all elastic does.
Signs that the brace may need replacing include the straps needing to be pulled much tighter than before to achieve the same sense of support; the brace feeling loose or less secure around the ankle despite correct fitting and an appropriate size; or visible damage to stitching, tears in the material, or a heel pad that no longer holds its basic shape.
The length of time the brace remains effective varies depending on how often and how long you wear it, the intensity of activities and conditions of use, and individual body size and how much load the brace is regularly carrying.
A worn brace may no longer limit roll and twist as effectively as it did when new. If you are unsure whether your brace is still offering adequate support, speak to a clinician about its role in your current management, and to the retailer if you have concerns about its condition.
30‑day FootReviver™ comfort and support guarantee
Choosing a semi‑rigid ankle brace is an important decision, particularly if you have had significant injuries or long‑standing symptoms.
To give you time to see how the FootReviver™ brace feels and functions in your usual walking and standing, it comes with a 30‑day money‑back guarantee. If, after trying it sensibly within this period, you find that the fit is not right for your ankle or footwear; it is not comfortable enough for the situations where your ankle usually feels at risk; or you do not feel it provides useful additional stability, you can arrange a return within 30 days for a refund.
This gives you time to see whether the brace suits you, especially if you have not used a semi‑rigid design before.
Is the FootReviver™ brace right for you?
When you do not trust your ankle, it can quietly narrow what you feel confident doing from day to day: how far you walk, which routes you choose, whether you use certain stairs, and which activities you start to avoid.
Across recurrent sprains, post‑fracture recovery, tendon problems and arthritis, the same mechanical issues tend to appear. Ligaments may no longer check side‑to‑side rolling as firmly as they once did. Tendons can be repeatedly strained at awkward angles around the heel. Joint surfaces often react badly to sudden twists and loads at the very end of movement. Many people describe this as having an “unstable ankle”.
The FootReviver™ Ankle Foot Orthosis Support Brace is designed in direct response to those realities. Its rigid metal side splints resist the rolling motions that so often cause sprains, tendon flare‑ups and sharp arthritic twinges. The open front and back allow the ankle to bend for walking so you can move more naturally, while still being protected from the extremes that cause trouble. The cupped padded heel section cushions impact and helps keep the heel more upright under the shin, influencing how force is spread through tendons, ligaments and joint surfaces. Wide adjustable straps and a padded interior aim to make this level of control both effective and tolerable during the times of day when your ankle does the most work.
Used alongside appropriate clinical advice, exercises to build strength and balance, and sensible decisions about activity and footwear, this brace can help everyday movement feel more secure and less dominated by fear of the ankle giving way or flaring painfully.
If you recognise your own ankle in these descriptions, and your clinician agrees that a brace is appropriate, the FootReviver™ brace is designed to give you that firmer sideways control without putting you back into a full boot. It is particularly aimed at people who can walk on level ground but do not yet feel safe when the surface tilts, becomes uneven or involves more stairs.
Before deciding, think about when your ankle usually struggles – uneven ground, longer periods standing, slopes, or the period after a cast or boot. Consider whether the semi‑rigid features outlined match your needs, as opposed to a lighter sleeve or a more rigid boot. Check the sizing guidance and whether you have footwear that can accommodate the brace if you intend to wear it in shoes. If you already have a specific type of support recommended by your clinician, compare that advice carefully with this design rather than substituting on your own.
If you are unsure, speaking to a GP, physiotherapist or podiatrist can help you decide whether this design fits into the plan you have agreed, and how best to use it if you choose to do so.
This product is intended for adult use only. Persistent, worsening or changing ankle or foot symptoms should always be discussed with a healthcare professional.
Disclaimer
The information on this page is general guidance for adults and does not replace individual medical advice, diagnosis or treatment. It describes typical ankle and foot problems and how this type of brace may support them, but it cannot take account of your full medical history or examination findings.
If you are unsure whether this brace is suitable for you, or if you have complex, persistent or changing symptoms, speak to a GP, physiotherapist, podiatrist or another appropriate clinician for personalised assessment and advice. No brace can guarantee specific results, and using a support should not delay seeking medical review when it is needed.
1 Review For This Product
Fast & Secure Checkout Through Paypal
Pay with Paypal the secure payment gateway that accepts all credit and debit cards. Paypal is free and secure and no credit or bank information is ever stored or shared with us.
Fast Dispatch
Enjoy your items soon with quick dispatch via Royal Mail. Expect to have your items between 1-3 working days for domestic orders. 7-10 Working days for international orders.
Return Policy – 30 Day Money Back Guarantee
In the unlikely event, you are unhappy with your purchase you can return it within 30 days for a refund. Please contact us via the form on the contact us page to start your return.
To return an item please send it to: Nuova Health UK, 81 Highfield Lane, Waverley, Rotherham, S60 8AL. Please include a note with your order id so we know who to refund. Please retain your postage receipt as proof of postage. All that we ask is that the item is in the original packaging and unused.



by Marian Rutter
Very good real support for my injured ankle highly recomend